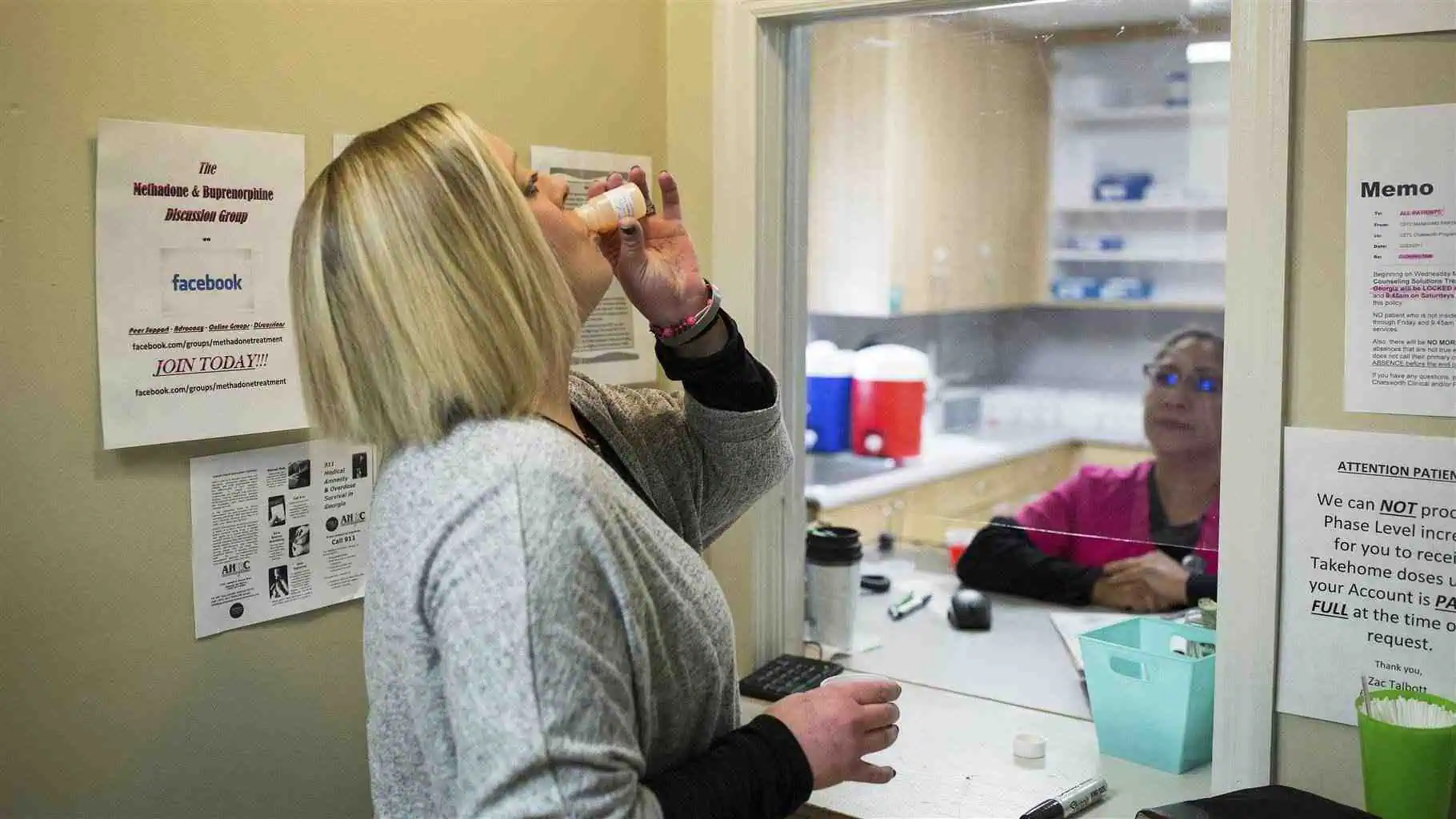
The journey to recovery really starts with a quiet, internal promise you make to yourself. It’s that moment you just know things have to change.
The Moment You Decide to Change
This isn’t always some dramatic, rock-bottom scene from a movie. More often, it’s a profound, gut-level realization that you’re ready to take your life back. It’s a feeling mixed with fear and a flicker of hope—the real turning point.
Instead of getting paralyzed by the long road ahead, the trick is to focus on what you can do right now. A little bit of structure at the very beginning goes a long way in cutting through the confusion and building some early confidence. You don’t have to have it all figured out. This is where your new life starts, one small, manageable decision at a time.
“Acknowledging you need help isn’t a sign of weakness. It’s the first and most courageous act of strength on the path to getting well. It’s the moment you choose yourself over your addiction.”
This process boils down to a few key things: admitting there’s a problem, reaching out for expert help, and starting to build healthier daily habits.
This image here breaks down the initial flow of recovery, showing a clear path from that first moment of awareness to taking real action.
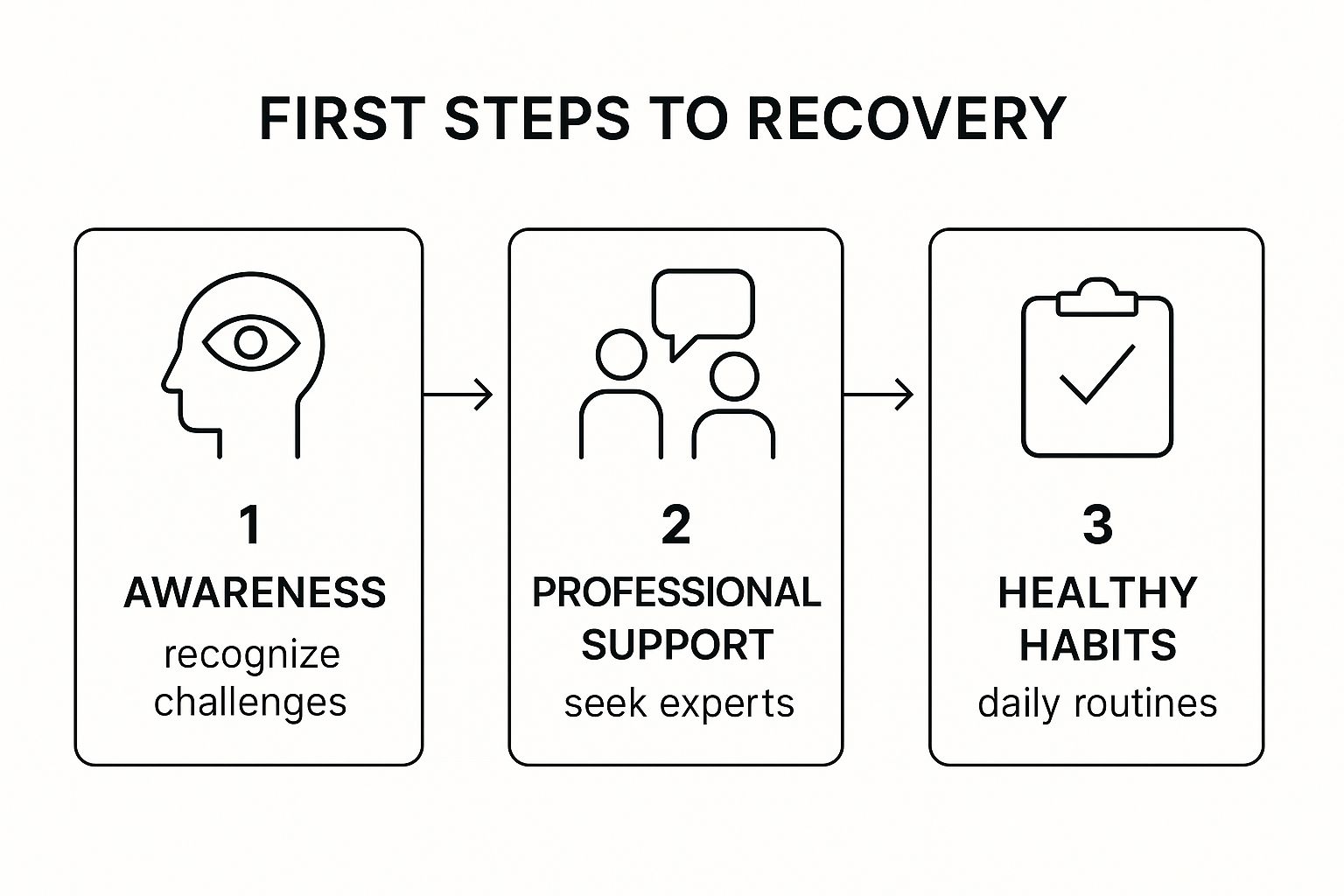
As you can see, recovery is a series of deliberate steps, not just one big leap. It all begins with that personal recognition and moves toward getting structured, professional support.
Understanding You Are Not Alone
It’s incredibly common to feel isolated when you’re struggling, but the truth is, you’re in a lot of company. The link between substance use and mental health is undeniable. For many, addiction starts as a way to self-medicate or cope with underlying emotional pain or an untreated mental health condition.
Think about it: worldwide, about 1 in 8 people live with a mental health disorder. That’s roughly 970 million individuals. The COVID-19 pandemic made things even tougher, contributing to a 26% jump in anxiety disorders and a 28% spike in major depressive disorders. Knowing this helps take the stigma out of what you’re going through and shows just how important it is to seek help. You can learn more about the global impact of mental health from the World Health Organization.
Your First 72 Hours Key Focus Areas
The first three days are absolutely critical for setting a positive tone for your recovery. By focusing on a few key priorities, you can build a solid foundation for safety and stability. This isn’t about solving everything at once, but about taking control of what you can, right now.
The table below breaks down these immediate priorities, helping you focus on what matters most in the first 72 hours.
| Priority Area | Immediate Action | Why It’s Important |
|---|---|---|
| Physical Safety | Contact a medical professional or detox facility to discuss safe withdrawal. | Withdrawal from certain substances can be dangerous or even fatal without medical supervision. Safety is the absolute first priority. |
| Building Support | Reach out to a trusted friend, family member, or a professional helpline. | Isolation fuels addiction. Making even one call breaks that isolation and starts the process of building a support network. |
| Creating Structure | Remove substances and paraphernalia from your environment. Plan your next 24 hours. | Immediate environmental changes reduce temptation and create a “clean slate.” A simple plan provides direction and a sense of purpose. |
| Emotional Honesty | Acknowledge your feelings without judgment. Write them down or share them with the person you contacted. | Recognizing and expressing your emotions is a fundamental step in addressing the root causes of addiction. It’s the beginning of emotional healing. |
Taking these initial steps creates a buffer of safety and support, giving you the breathing room you need to start the deeper work of healing.
When you’re ready to start recovery, the first order of business is your physical health. Let’s be blunt: for many substances, trying to detox cold turkey on your own isn’t just hard—it can be downright dangerous. Withdrawal is a serious medical event, and getting through it safely isn’t a sign of weakness. It’s the smartest, safest first step you can take.

The word “detox” can bring up some scary images, but the reality is much different. A medically supervised detox is a controlled, supportive environment designed to manage your withdrawal symptoms and keep you as comfortable and safe as possible. Think of it as stabilizing your body so the real work of emotional healing can begin.
Call Now – Your Journey to Recovery Begins Today!

Take the first step towards a healthier life! Call now to connect with our compassionate team and start your recovery journey today. Your path to healing awaits!
Our recovery specialists are available 24/7 to provide support, and all calls are confidential and free. Reach out anytime – we’re here to help!
What Really Happens During Detox
Whether you check into a facility or use an outpatient clinic, the goal is the same: to help your body safely clear itself of substances while being monitored by medical professionals. This isn’t about gritting your teeth and “toughing it out.” It’s about using medical science and expert care to make the process manageable.
For instance, withdrawal from alcohol or benzodiazepines can trigger life-threatening complications like seizures or delirium tremens (DTs). In a professional facility, clinicians will monitor your vital signs—like your heart rate and blood pressure—around the clock.
“The purpose of medical detox is not to punish, but to protect. It’s the bridge that gets you from physical dependence to the emotional and psychological work of recovery, ensuring you arrive safely.”
They are trained to spot warning signs and can administer specific medications to prevent these severe outcomes and make you more comfortable. This approach dramatically increases your safety and your chances of actually completing detox and moving forward.
Inpatient vs. Outpatient: What’s Right for You?
The choice between an inpatient and outpatient detox really comes down to your unique situation. You’ll want to consider the substance you’ve been using, how long you’ve been using it, and what your home life is like.
- Inpatient Detox: This is where you live at the facility 24/7, getting constant medical care and support. It’s by far the safest option if you have a significant physical dependency or if your home environment isn’t stable or substance-free. It completely removes you from triggers and access.
- Outpatient Detox: With this option, you live at home but visit a clinic or hospital daily for check-ups and medication. This can work well for people with milder withdrawal symptoms and a very strong, sober support system at home. It offers more flexibility but demands a huge amount of personal discipline.
An addiction specialist is the best person to help you make this call. They can perform an assessment and recommend the level of care that will give you the strongest foundation for lasting recovery.
The Role of Medication in a Safe Detox
Medication is one of the most powerful tools for a safe and successful detox. This is a core component of what’s known as medication-assisted treatment (MAT), a proven method that combines FDA-approved medications with counseling and therapy.
For opioid withdrawal, medications like buprenorphine can significantly reduce cravings and ease the worst of the symptoms. For alcohol withdrawal, certain medications can prevent deadly seizures and keep your body stable. It’s critical to understand that this is not about “replacing one drug with another.” To get the full picture, you can explore this detailed explanation of what medication-assisted treatment involves and see how it supports long-term success. These are carefully prescribed and monitored treatments designed to manage the acute physical crisis of withdrawal.
How to Choose a Reputable Provider
Finding the right treatment provider is one of the most important decisions you’ll make. Not all detox centers are created equal, and you need to do a little homework to find a place that’s credible and feels right for you.
When you start calling potential facilities, come prepared with a list of questions. This is your health and your future—you have every right to be a thorough consumer.
Questions to Ask a Potential Detox Facility
| Category | Specific Question to Ask | Why It Matters |
|---|---|---|
| Licensing & Accreditation | “Are you licensed by the state and accredited by a national body like The Joint Commission or CARF?” | This proves they meet high standards for safety and quality of care. |
| Medical Staff | “What kind of medical staff do you have on-site 24/7? Are there doctors and registered nurses?” | You need to know that qualified medical experts are available at all times, not just on call. |
| Treatment Approach | “What is your specific protocol for the substance I’ve been using? What medications do you typically use?” | A legitimate provider will have a clear, evidence-based plan tailored to your specific situation. |
| Aftercare Planning | “What happens when detox is over? How do you help me transition to the next step in recovery?” | Detox is just the beginning. A good facility will already be planning your next move to ensure you don’t fall through the cracks. |
Be on the lookout for red flags. These include promises of a “guaranteed cure,” high-pressure sales tactics, or vague, evasive answers about their staff and licensing. A quality provider will be transparent, compassionate, and focused on setting you up for long-term well-being. Asking these questions will empower you to make a confident, informed decision for your health.
How to Build Your Real-World Support System
Getting through detox and finding your physical footing is a huge win. Seriously, take a moment to acknowledge that. But now, the real work begins—building the human foundation that will support you through the emotional ups and downs of recovery.
You can’t do this alone. And the best part is, you don’t have to. Assembling a reliable support system is one of the most powerful moves you can make to safeguard your sobriety.

This isn’t just about telling your family you’ve quit. It’s about being strategic. It’s about being intentional with who you let into your inner circle and what role they’ll play. Real support is an active, ongoing mix of connection, raw honesty, and crystal-clear boundaries.
Having the Conversation with Family and Friends
Telling the people closest to you can feel absolutely terrifying. You’re probably worried about judgment, disappointment, or just fumbling the words. My advice? Keep it simple, keep it honest, and focus on what you need from them now.
You don’t owe anyone a dramatic, tear-filled confession or a play-by-play of your past. A straightforward approach almost always works best. Try something like, “I’m working on getting healthy and have decided to stop drinking. Your support and understanding would mean the world to me as I figure this out.”
“The point of this talk isn’t to get forgiveness or a round of applause. It’s to set new rules of engagement for the relationship—ones that put your recovery first, no exceptions.”
This simple script puts you back in the driver’s seat. It makes it clear that your recovery is a non-negotiable part of your life and tells them exactly how they can help you win.
Differentiating Support from Enabling
Here’s where it gets tricky. Involving loved ones means learning to spot the thin line between genuine help and enabling. Enabling almost always comes from a good place—from love—but it ultimately insulates you from the consequences of your actions, which is a disaster for recovery.
Making sure everyone understands the difference is a game-changer.
- What Support Looks Like: Encouraging you to hit a meeting, respecting your request to not have alcohol in the house, listening without jumping to conclusions, and celebrating your wins, big or small.
- What Enabling Looks Like: Making excuses for you, giving you cash you might use on substances, or telling you a near-relapse “wasn’t a big deal.”
Firm boundaries are your only defense against enabling. It is perfectly okay to say, “I can’t be around drinking right now, so I’m going to skip the party. How about we grab coffee next week instead?” This isn’t about punishing anyone; it’s about protecting yourself.
Call Now – Your Journey to Recovery Begins Today!

Take the first step towards a healthier life! Call now to connect with our compassionate team and start your recovery journey today. Your path to healing awaits!
Our recovery specialists are available 24/7 to provide support, and all calls are confidential and free. Reach out anytime – we’re here to help!
Finding Your People in Peer Groups
Family and friends are one thing, but there’s a unique power in connecting with people who have walked in your shoes. Peer support groups offer a kind of understanding that no one else can quite grasp. For many, they are the bedrock of a lasting recovery. The data is clear: consistent engagement with peer groups is strongly tied to long-term abstinence.
You’ve got a few solid, evidence-based options, each with its own vibe:
- Alcoholics Anonymous (AA) and Narcotics Anonymous (NA): These are the 12-step programs you’ve likely heard of. They’re built on a spiritual framework that involves working the steps with a sponsor.
- SMART Recovery: This is a more secular, science-backed alternative. It uses tools from cognitive-behavioral therapy (CBT) to help you manage your thoughts and behaviors, focusing on self-empowerment.
The only way to know what fits is to try them out. You can explore a variety of support groups for addiction to see which philosophy and community feels right. Your first meeting might feel awkward. That’s normal. Just go, sit, and listen. You’ll eventually hear pieces of your own story in someone else’s, and that’s where the magic starts.
The right support system is your safety net. It’s a mix of professional help, an informed family, and peers who just get it. Building this team is one of the most critical moves you’ll make.
Understanding the Roots of Your Addiction
Once your body is physically stable after detox, the real work begins. This is where you move beyond the what of your addiction and start digging into the why. Honestly, discovering the reasons behind your substance use is one of the most critical steps in recovery. It’s the key to building a sobriety that actually lasts.

For so many people I’ve worked with, addiction isn’t the core problem—it’s a symptom. It often starts as a way to cope with or numb the pain of something deeper, like anxiety, depression, or past trauma. In the professional world, we call this a co-occurring disorder or a dual diagnosis.
Your mental health is the true foundation of your recovery. If you only treat the substance use without getting to the bottom of the emotional pain driving it, you’re only solving half the puzzle. It’s like patching a leaky roof over and over without ever fixing the hole that’s causing the leak in the first place.
The Connection Between Addiction and Mental Health
The link between substance use and other mental health conditions is incredibly strong—think of them as two sides of the same coin. For instance, someone struggling with crippling social anxiety might start drinking to feel more comfortable in social settings. Over time, that coping mechanism can easily spiral into a full-blown dependency. For a closer look at this specific pattern, our guide to understanding alcohol addiction offers some valuable insights.
This connection isn’t just personal; it’s a massive global challenge. Mental health conditions contribute to a staggering 290 million disability-adjusted life years worldwide. Yet, these conditions often receive only about 2% of government healthcare funding, creating a massive gap in care.
Finding a Therapist Who Gets It
Working with a mental health professional is non-negotiable for untangling these roots. But let me be clear: not just any therapist will do. You need someone who specializes in both addiction and co-occurring disorders.
Here’s what to look for when finding the right person:
- Check for Credentials: Look for therapists with certifications like “Licensed Alcohol and Drug Counselor” (LADC) or similar titles that show they have specialized training.
- Ask About Their Approach: Inquire if they use proven methods like Cognitive Behavioral Therapy (CBT) or Dialectical Behavior Therapy (DBT), which are highly effective for addiction and emotional regulation.
- Trust Your Gut: A good therapeutic relationship is built on trust and safety. During an initial consultation, ask yourself: Do I actually feel seen and heard by this person?
“Your first few therapy sessions aren’t about digging up your most painful memories. They’re about building a connection, establishing a sense of safety, and figuring out some goals. It’s a space where you can finally start talking without the fear of judgment.”
The initial goal is simply to create a safe container for your story. Your therapist will guide you in understanding your triggers, developing healthier ways to cope, and slowly processing any underlying issues at a pace that feels right for you.
Gentle First Steps for Emotional Awareness
While therapy is a cornerstone, you can also start building emotional awareness on your own with a few simple, gentle practices. These techniques help you connect with your feelings without getting completely overwhelmed.
Journaling Prompts to Get You Started:
- “Today, I felt [emotion] when [event] happened. In my body, it felt like…”
- “What is one small thing I did just for my well-being today?”
- “A feeling I tend to avoid is… Why do I think that is?”
Mindfulness is another powerful tool. This isn’t about emptying your mind—it’s about paying attention to right now, without judgment.
Try this simple two-minute exercise:
- Find a quiet spot and sit comfortably.
- Close your eyes and just focus on the sensation of your breath coming in and going out.
- When your mind wanders (and it definitely will), gently notice the thought and guide your focus back to your breath. No need to get frustrated—it’s part of the practice.
These small, consistent actions build your “muscle” for emotional regulation. They teach you that you can sit with a difficult feeling without immediately needing to numb or escape it. This self-awareness is where true healing takes root, turning your first steps into a sustainable, lifelong journey.
Call Now – Your Journey to Recovery Begins Today!

Take the first step towards a healthier life! Call now to connect with our compassionate team and start your recovery journey today. Your path to healing awaits!
Our recovery specialists are available 24/7 to provide support, and all calls are confidential and free. Reach out anytime – we’re here to help!
Creating a Daily Routine That Supports Sobriety
Early recovery is a time of massive upheaval. You’re not just stopping a behavior; you’re fundamentally rewiring your life, swapping out old, destructive habits for new, positive ones. The single most powerful tool you have during this time is structure. A predictable daily routine becomes your guardrail, keeping you on track when cravings, boredom, or tough emotions show up uninvited.
This isn’t about creating a rigid, military-style boot camp for yourself. Far from it. The goal is to build a simple, repeatable framework for your day that puts your well-being first. Think of it this way: addiction loves chaos and spontaneity. Sobriety, on the other hand, thrives on consistency and purpose. By planning your days, you’re making a conscious choice—over and over again—to prioritize your recovery.
This structure takes the guesswork out of your day, reducing decision fatigue and freeing up precious mental energy for the real work: healing.
Fuel Your Body to Stabilize Your Mind
What you eat has a direct and immediate impact on your mood, energy, and cravings. In early recovery, your body is working overtime to heal itself. One of your best allies in this fight is stable blood sugar. It helps fend off the emotional roller coaster that can easily trigger the urge to use.
You don’t have to become a gourmet chef overnight. Simple meal planning is a fantastic starting point. The real aim is just to eat regular, balanced meals to sidestep the energy crashes and mood swings that make you vulnerable.
- Plan Three Meals: Aim to eat breakfast, lunch, and dinner at roughly the same time each day. Consistency is key.
- Prioritize Protein: Make sure every meal has a good source of protein—think eggs, chicken, beans, or tofu. It keeps you feeling full and your energy levels steady.
- Stay Hydrated: It’s so simple, but so many of us forget it. Dehydration can masquerade as hunger or even a craving. Keep a water bottle with you and make it a habit to sip throughout the day.
This focus on nutrition isn’t just about physical health. It’s a foundational act of self-care. Every balanced meal is a small but powerful statement that you are worth the effort.
The Importance of Movement and Sleep
Physical activity is one of the most potent, non-medical tools in your recovery arsenal. You don’t need to sign up for a marathon. Gentle, consistent movement is what truly matters. Exercise releases endorphins natural mood elevators and helps burn off the restless, anxious energy that plagues so many in early sobriety.
“A 20-minute walk can do more for a bad mood than an hour of stewing in your own thoughts. Movement gets you out of your head and into your body, breaking the cycle of negative thinking.”
Sleep is just as critical. It’s when your brain does its most important repair work. A consistent sleep routine is non-negotiable for healing. Try to go to bed and wake up around the same times each day, even on weekends. A simple “wind-down” ritual—like reading a chapter of a book or listening to some calm music—can be a powerful signal to your brain that it’s time to shut down and recharge.
Fill the Void with Healthy Pursuits
Let’s be honest: addiction took up a lot of time, energy, and mental real estate. Now that it’s gone, you might be staring into a pretty significant void. It is absolutely crucial to fill that space with new, fulfilling activities. This is your chance to rediscover who you are—or discover who you want to become—outside the context of substance use.
Start small. Make a simple list of things you used to enjoy before addiction took over, or things you’ve always been curious about trying. The goal is to find activities that genuinely engage your mind and spirit, giving you a sense of joy and purpose.
Ideas for New Hobbies:
- Creative: Learn a few chords on a guitar, take up painting, or just start a simple journal to get your thoughts out.
- Active: Explore local hiking trails, join a casual sports league, or get your hands dirty with some gardening.
- Mindful: Give yoga or meditation a try. Even something as simple as bird-watching can be an incredible practice in mindfulness.
These activities aren’t just ways to kill time; they are the literal building blocks of a new, sober life. As you weave these elements into a daily routine, you’re not just avoiding the old life—you’re actively building a new one that you won’t want to escape from.
Remember, building a solid routine is a core part of long-term success. You can find more strategies in our comprehensive guide on aftercare and relapse prevention, which dives deeper into maintaining sobriety for the long haul. A life you love is your best defense.
Call Now – Your Journey to Recovery Begins Today!

Take the first step towards a healthier life! Call now to connect with our compassionate team and start your recovery journey today. Your path to healing awaits!
Our recovery specialists are available 24/7 to provide support, and all calls are confidential and free. Reach out anytime – we’re here to help!
Answering Your Questions About Starting Recovery
Taking that first step toward getting sober is huge, but it also kicks up a storm of questions and “what-ifs.” Feeling a little lost or uncertain right now is completely normal. Having some straight answers can help quiet that noise in your head and give you the confidence you need to move forward.
Let’s break down some of the biggest concerns people have when they first start their recovery journey.
What Happens If I Relapse?
First, let’s get one thing straight: relapse is not a moral failing. It’s not a sign that you can’t do this. So many people experience a setback on their way to long-term sobriety. The best way to look at it is as a signal—a moment that shows you something in your plan needs a tune-up. It’s a chance to spot a new trigger and strengthen your recovery with what you’ve just learned about yourself.
The most critical thing to do after a relapse is to reach out for help immediately. Don’t wait. Call your sponsor, therapist, or someone you trust from your support group. Shame and guilt are powerful forces that will try to push you back into isolation, which is the last place you need to be. Being honest in that moment is your greatest strength.
“A relapse doesn’t erase the progress you’ve made. It’s a painful detour, but it doesn’t have to be the end of the road. The real failure would be giving up on yourself entirely.”
How Should I Tell My Family and Friends?
This is a tough one, and it’s all about setting boundaries and clearly asking for the right kind of support. This conversation isn’t about confessing or begging for approval. It’s about stating your needs.
Find a calm, private moment to talk. You can be direct without giving them every last detail of your past. Something simple like, “I’m making a big change for my health and I’ve decided to stop using. What I really need from you right now is your patience and support as I figure this out,” works wonders. This approach puts you in control and sets a clear, healthy expectation.
For a deeper dive, our article on how to help a drug addict has some great tips that can help both you and your loved ones navigate this important talk.
How Much Does Treatment Cost?
The cost of addiction treatment really runs the gamut. It depends on everything from the level of care (like inpatient versus outpatient) to the facility’s location and how long the program is. The good news is, many treatment centers accept private health insurance, which can dramatically lower what you have to pay out-of-pocket.
Here are a few practical steps to figure it out:
- Call Your Insurance Provider: This is your first move. Get on the phone with your insurance company and ask them to explain your benefits for mental health and substance abuse treatment.
- Ask Centers About Payment Options: When you call a facility, don’t be shy. Ask if they offer payment plans or sliding-scale fees that are based on your income.
- Look into Publicly-Funded Programs: Check out state-funded programs in your area. They often provide services that are low-cost or even free.
Getting access to quality mental health care can feel like an uphill battle, which makes taking the first steps to recovery even harder. A recent WHO guidance on transforming mental health policies showed that in some countries, up to 90% of people with serious conditions get no care at all. Don’t let the fear of cost stop you before you start. Resources are out there if you know where to look.
If you or someone you care about is ready to take the first steps to recovery, help is here. At Addiction Helpline America, we connect you with compassionate, trusted professionals who can guide you toward a healthier future. Contact us today to start your journey.
Our helpline is 100%
free & confidential
If you or someone you care about is struggling with drug or alcohol addiction, we can help you explore your recovery options. Don’t face this challenge alone—seek support from us.
Programs
Resources
Will my insurance
cover addiction
treatment?
We're ready to help
Find the best
drug or alcohol treatment
center
Are you or a loved one struggling with addiction? Call today to speak to a treatment expert.