
The Unseen Struggle of Opioid Withdrawal
Signs, Symptoms, and Withdrawal (Consolidated) encompass both physical and emotional reactions when someone stops using opioids after regular use. Understanding these symptoms can be life-saving for those affected by opioid use disorder.
Quick Overview of Opioid Withdrawal:
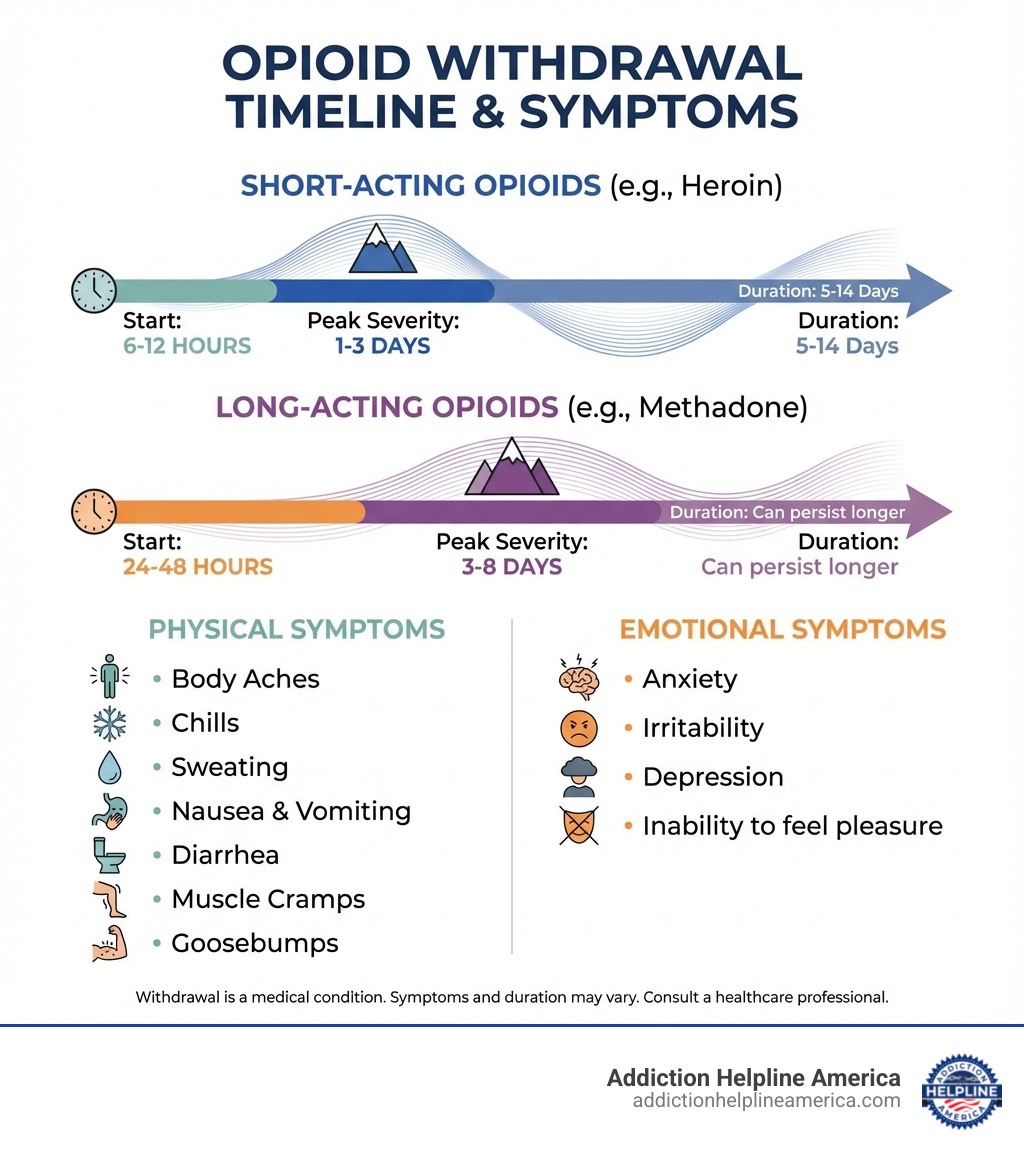
- Physical symptoms include body aches, chills, sweating, nausea, vomiting, diarrhea, muscle cramps, and goosebumps
- Emotional symptoms include anxiety, irritability, depression, and inability to feel pleasure
- Timeline varies based on the opioid type: short-acting opioids (like heroin) cause symptoms within 6-12 hours, while long-acting opioids (like methadone) may take 24-48 hours
- Peak severity typically occurs within 1-3 days for physical symptoms
- Duration ranges from 5-14 days, though emotional symptoms can persist longer
- Not life-threatening for opioids alone, but extremely uncomfortable and drives continued drug use
The scale of this crisis in the United States is staggering. Millions of Americans are affected by opioid use disorder (OUD), and in 2021 alone, over 80,000 people died from opioid-related overdoses. Behind each statistic is a person struggling with withdrawal’s powerful grip.
Withdrawal happens because your body has adapted to the presence of opioids. When you stop using them, your brain and body rebel. The symptoms oppose the initial euphoric effects that drugs once provided. Instead of feeling good, you feel terrible—physically sick and emotionally devastated.
But here’s the critical truth: withdrawal is a medical condition, not a moral failing. Understanding what’s happening in your body and brain is the first step toward recovery. Treatment exists. Help is available. Recovery is possible.
At Addiction Helpline America, we’ve guided thousands of individuals and families through understanding signs, symptoms, and withdrawal (consolidated) to find appropriate treatment programs. Our free, confidential service connects you with evidence-based care custom to your specific situation—call us 24/7 at 844-561-0606.
Understanding Opioid Withdrawal: The Two Sides of Symptoms
Withdrawal is your body’s intense reaction to the absence of a substance it has become dependent on. Imagine your body trying to rebalance itself after being accustomed to a constant stream of opioids. This process is far from pleasant, often characterized by a cascade of aversive symptoms that starkly contrast the initial rewarding and euphoric effects of drug use. The experience manifests as a complex interplay between physical discomfort and emotional distress, creating a challenging environment for anyone attempting to cease opioid use.

Physical (Somatic) Symptoms: The Body’s Protest
When we talk about the signs, symptoms, and withdrawal (consolidated) experience, the physical manifestations are often the most recognized. These somatic symptoms are what many people describe as feeling like an extreme flu. They can be incredibly debilitating, making even simple daily tasks feel impossible.
Typical somatic signs of opioid withdrawal include:
- Body Aches: A deep, generalized pain throughout the muscles and joints.
- Chills and Hot Flashes: Rapid shifts in body temperature, often accompanied by sweating.
- Gastrointestinal Upset: Severe nausea and vomiting, often leading to dehydration.
- Diarrhea: Frequent and often painful bowel movements.
- Hyperalgesia: An increased sensitivity to pain, making even light touch unbearable.
- Piloerection (Goosebumps): The skin’s tiny muscles contract, causing hair to stand on end, a classic sign often referred to as “cold turkey.”
- Pupil Dilation: Enlarged pupils, even in normal lighting conditions.
- Lacrimation and Rhinorrhea: Excessive tearing and a runny nose, respectively.
- Yawning: Frequent and uncontrollable yawning.
The timeline for these physical symptoms can vary significantly. For short-acting opioids like heroin, symptoms typically begin within 6-12 hours of the last dose and reach their peak intensity within 1-3 days. For longer-acting opioids such as methadone, the onset might be delayed to 24-48 hours, with peak symptoms occurring anywhere from 3 to 8 days. While these physical symptoms are profoundly uncomfortable, they are generally not life-threatening on their own. However, the sheer discomfort can be a powerful driver for continued drug use, making medically-supervised detox an essential step towards recovery.
Emotional (Affective) Symptoms: The Mind’s Struggle
While physical symptoms are undeniable, the emotional or affective signs, symptoms, and withdrawal (consolidated) are arguably more critical in driving and perpetuating opioid addiction. These symptoms impact an individual’s mental and emotional well-being, creating a deeply negative internal state that makes abstinence incredibly difficult.
Key affective signs of opioid withdrawal include:
- Anxiety: Intense feelings of worry, nervousness, or unease.
- Irritability: Heightened frustration and a short temper.
- Anhedonia (Inability to Feel Pleasure): A profound loss of interest or pleasure in activities that were once enjoyable. This can make natural rewards feel dull and unappealing.
- Reduced Motivation: A significant decrease in the drive to engage in daily activities, pursue goals, or interact with others.
- Psychological Distress: A general feeling of misery, despair, and emotional turmoil.
Research indicates that these affective signs are not merely secondary to physical discomfort; they play a significant, if not more significant, role in addiction. Affective withdrawal symptoms can be observed even after just one or a few opioid exposures and tend to intensify with continued drug use. This negative affective state, a form of heightened emotional distress, actively promotes drug-seeking behavior and relapse. The brain, seeking relief from this intense emotional pain, directs all its efforts toward acquiring the drug that will alleviate it.
Understanding the profound impact of these emotional symptoms is crucial for effective treatment. Addressing the psychological distress is just as important as managing the physical discomfort. For more comprehensive information on treatment approaches that tackle both the physical and emotional aspects of opioid addiction, explore our resources on opioid addiction treatment.
The Vicious Cycle: How Withdrawal Fuels Addiction
The experience of opioid withdrawal is not just a temporary discomfort; it’s a powerful force that traps individuals in the cycle of addiction. This cycle is driven by a fundamental shift in motivation, moving from seeking the pleasure of the drug to desperately avoiding the pain of its absence.
Negative Reinforcement: The Addiction Trap
Initially, people might use opioids for their euphoric effects or to manage pain. However, as dependence develops, the motivation shifts dramatically. The driving force becomes negative reinforcement—the desire to escape or avoid the unpleasant signs, symptoms, and withdrawal (consolidated). The drug is no longer primarily about getting “high”; it’s about not getting “sick.” This is the core of the addiction trap. The brain learns that taking the drug provides immediate relief from withdrawal, thus reinforcing the drug-seeking behavior. Opioid withdrawal plays a central and critical role in maintaining the addiction cycle.
The Brain’s Memory of Discomfort: Conditioned Withdrawal
One of the most insidious aspects of withdrawal is its ability to become “conditioned.” This means that environmental cues—people, places, things, or even emotions—that were present during past drug use or withdrawal can themselves trigger withdrawal-like symptoms, even in the absence of the drug. This phenomenon, known as conditioned withdrawal, is a powerful driver of relapse.
Imagine someone who always used opioids in a particular room. Even after abstaining for some time, simply entering that room can evoke intense cravings and physiological responses akin to actual withdrawal. This is because the brain has formed strong associations, or memories, between the environment and the drug experience.
Research, including studies on “Extended amygdala, conditioned withdrawal and memory consolidation,” highlights how this process works. Conditioned withdrawal is believed to perpetuate the addiction cycle by strengthening the storage of memories associated with drug-seeking behaviors. When an individual experiences conditioned withdrawal, the brain reinforces the memory that taking the drug is the solution to this distress, making relapse more likely. This happens through a process called memory consolidation, where withdrawal states improve the permanence of these drug-associated memories. You can dig deeper into the scientific understanding of this complex interaction by reading scientific research on conditioned withdrawal and memory.
The Anti-Reward System: A Brain in Turmoil
Chronic opioid use and repeated cycles of withdrawal lead to profound alterations in the brain’s reward circuitry. What was once a system designed to motivate us towards natural rewards (food, water, social connection) becomes dysregulated. This shift is often described as the activation of an “anti-reward system.”
Instead of experiencing pleasure, individuals in withdrawal experience a state of intense dysphoria—a severe negative emotional state characterized by heightened distress. The brain’s stress systems become hyperactive, further contributing to this negative state. This “dark side” of addiction means the brain is no longer primarily seeking pleasure; it’s desperately trying to alleviate suffering. This constant internal turmoil makes it incredibly difficult to resist drug-seeking behaviors.
Understanding this shift is crucial for effective treatment, as it underscores the need to address the deep-seated neurobiological changes that occur with addiction. Finding the right treatment program that can help steer these complex brain changes is a vital step toward reclaiming a life free from addiction. If you or a loved one are struggling, our helpline offers free, confidential guidance to help you find a treatment program that addresses these intricate challenges.
The Science Behind the Struggle: Key Brain Systems in Withdrawal
The profound and distressing signs, symptoms, and withdrawal (consolidated) are not random; they are the result of complex neurobiological changes within the brain. Chronic opioid exposure leads to significant adaptations, essentially rewiring the brain to depend on the drug. When the opioid is removed, these adapted systems go into overdrive, creating a state of hyperexcitability and distress. Understanding these underlying mechanisms is crucial for developing effective treatments and offering genuine hope for recovery.
The Role of the Amygdala and Stress Systems in Signs, Symptoms, and Withdrawal (Consolidated)
At the heart of the emotional and motivational aspects of opioid withdrawal lies the extended amygdala (EA). This critical brain region is not a single structure but a network comprising the central amygdala (CeA), the bed nucleus of the stria terminalis (BNST), and the nucleus accumbens shell (NAcc shell). These interconnected areas share similar characteristics and play a pivotal role in mediating negative emotional states, stress responses, and memory consolidation related to withdrawal.
When opioids are chronically present, and then suddenly withdrawn, this extended amygdala becomes highly active. This hyperactivity contributes significantly to the negative affective symptoms we discussed earlier, such as anxiety, dysphoria, and irritability. A key player in this stress response is Corticotropin-Releasing Factor (CRF), a neuropeptide that becomes dysregulated during withdrawal. Increased CRF activity within the extended amygdala, particularly in the CeA and BNST, drives the aversive emotional states.
Furthermore, the entire hypothalamic-pituitary-adrenal (HPA) axis, our body’s central stress response system, becomes hypersensitive during opioid withdrawal. Studies show increased levels of stress hormones like cortisol and ACTH (adrenocorticotropic hormone) in both rodents and humans during withdrawal. This heightened stress response is also reflected in increased plasma concentrations of epinephrine and norepinephrine (NE), which contribute to many of the physical and emotional symptoms, such as increased heart rate, blood pressure, and anxiety. The intricate neuroplastic changes within the extended amygdala during opioid withdrawal and prolonged abstinence are areas of active research, as highlighted in Neuroplasticity of the extended amygdala in opioid withdrawal.
Changes in the Brain’s Reward and Alertness Centers
Beyond the extended amygdala, other crucial brain systems undergo significant alterations that contribute to the comprehensive signs, symptoms, and withdrawal (consolidated).
-
Mesolimbic Dopamine System: This system is often referred to as the brain’s “reward pathway,” but its function is far more complex than just pleasure. It plays a key role in motivation, learning, and incentive salience—making certain cues and actions highly desirable. During chronic opioid use, this system adapts. However, during withdrawal, there’s often a profound decrease in dopamine function, particularly in the nucleus accumbens. This decreased dopamine activity is thought to underlie the anhedonia (inability to feel pleasure) and reduced motivation experienced during withdrawal. The brain struggles to find joy in natural rewards, making the artificial “reward” of opioid relief even more compelling.
-
Locus Coeruleus (LC) Hyperactivity: The locus coeruleus is a small but powerful brain nucleus that acts as the primary source of norepinephrine (NE) in the brain. NE is involved in alertness, arousal, and stress responses. During opioid withdrawal, the LC becomes hyperactive. This surge in NE release contributes significantly to many of the classic physical withdrawal signs, such as sweating, tremors, rapid heart rate, and gastrointestinal distress. It also fuels the anxiety, agitation, and general state of hyperarousal that makes withdrawal so unbearable. The hyperactivity of the LC is a major contributor to the acute somatic symptoms.
These intricate changes in various brain regions demonstrate that opioid withdrawal is a deeply ingrained physiological and psychological process, explaining the immense challenge individuals face during detoxification.
Factors Influencing the Severity of Signs, Symptoms, and Withdrawal (Consolidated)
The experience of opioid withdrawal is rarely identical for any two individuals. It’s a highly personalized journey, influenced by a multitude of factors that can significantly impact the intensity and duration of signs, symptoms, and withdrawal (consolidated). Understanding these individual differences is crucial for tailoring effective treatment plans and providing compassionate care.
Individual Differences and Patterns of Use
Several key elements contribute to the unique profile of a person’s withdrawal experience:
- Type of Opioid: Different opioids have varying half-lives, which directly affects the onset and duration of withdrawal. Short-acting opioids (e.g., heroin, fentanyl) typically lead to rapid-onset, intense, but shorter-lived withdrawal. Long-acting opioids (e.g., methadone, buprenorphine) result in a delayed onset but a more protracted and often less acute withdrawal syndrome.
- Duration and Dosage: The longer an individual has used opioids and the higher the daily dose, the more severe their physical dependence is likely to be, leading to more intense and prolonged withdrawal symptoms.
- Intermittent vs. Continuous Use: Interestingly, the pattern of drug exposure can also play a role. Intermittent opioid administration, which involves cycles of use followed by periods of withdrawal, can lead to a greater abuse liability than continuous administration. This is because the brain repeatedly experiences the aversive withdrawal state, reinforcing the drive to seek the drug for relief.
- Co-occurring Health Conditions: Individuals with underlying physical or mental health conditions may experience more complicated or severe withdrawal. For example, chronic pain can be exacerbated, and anxiety disorders can intensify during opioid withdrawal.
- Genetic Factors: Emerging research suggests that genetic predispositions can influence an individual’s vulnerability to developing opioid dependence and the severity of their withdrawal symptoms.
These factors highlight why a “one-size-fits-all” approach to detox and treatment is often ineffective. Personalized care, beginning with a thorough assessment of an individual’s history and current health, is paramount. For those seeking safe and effective ways to manage withdrawal, exploring various detox programs is a critical first step.
Are There Sex Differences in Opioid Withdrawal?
The question of sex differences in addiction and withdrawal is an important area of ongoing research. While historically, much of the addiction research has focused on male subjects, a growing body of evidence suggests that men and women may experience signs, symptoms, and withdrawal (consolidated) differently, both behaviorally and neurologically.
- Symptom Severity: Some studies indicate that there might be sex differences in the expression and severity of withdrawal symptoms. For instance, preclinical research in rodents has shown that male rodents often exhibit greater somatic (physical) signs of morphine withdrawal compared to females. This could potentially be linked to differences in how pain is modulated in the brain, particularly in areas like the periaqueductal gray (PAG).
- Neural Mechanisms: The underlying neural mechanisms mediating withdrawal may also differ between sexes. Hormonal influences (e.g., estrogen, progesterone) can impact opioid receptor function and the activity of stress-related brain circuits.
- Implications for Treatment: Recognizing these potential sex differences is vital for developing more effective and personalized treatment strategies. What works best for one sex might not be optimal for the other. For example, understanding how hormonal fluctuations might influence withdrawal severity in women could lead to more custom pharmacological or behavioral interventions.
The field is actively working to address the historical underrepresentation of female subjects in addiction research to gain a more complete picture. As our understanding of these nuances grows, we move closer to a truly personalized approach to addiction medicine, ensuring that treatment is as effective as possible for everyone.
Finding a Path Forward: Treatment and Hope for Recovery
The journey through withdrawal can feel overwhelming and isolating, a dark tunnel with no end in sight. But we want to assure you that recovery is not just a dream; it’s a tangible reality for countless individuals. Understanding the signs, symptoms, and withdrawal (consolidated) is a powerful first step, but it’s equally important to know that you don’t have to face it alone. Professional help is not just beneficial; it’s often essential, providing the safety, support, and medical expertise needed to steer this challenging period.
Medically-Supervised Detox and Support
Attempting to detox from opioids without medical supervision can be dangerous and is often unsuccessful due to the intensity of withdrawal symptoms. Medically-supervised detox provides a safe and supportive environment where your physical and emotional well-being can be closely monitored.
Key components of medically-supervised detox include:
- Safety and Comfort: Medical professionals can manage uncomfortable and potentially risky symptoms, ensuring your safety throughout the process.
- Managing Symptoms: Medications are often used to alleviate the severity of withdrawal symptoms, making the process more tolerable and increasing the chances of successful detoxification.
- Medications for Opioid Use Disorder (MOUD): These medications are cornerstones of modern addiction treatment, helping to stabilize individuals and prevent relapse.
- Buprenorphine: A partial opioid agonist that reduces withdrawal symptoms and cravings without producing the same euphoric effects as full opioids.
- Methadone: A full opioid agonist that prevents withdrawal and reduces cravings, often administered in highly regulated clinics. Methadone maintenance therapy is considered a gold-standard treatment for OUD.
- Naltrexone: An opioid antagonist that blocks the effects of opioids, preventing relapse by eliminating the reward associated with opioid use.
These pharmacological maintenance therapies are highly effective in preventing withdrawal symptoms and supporting long-term abstinence. They work by addressing the underlying neurobiological changes caused by opioid dependence. If you or someone you care about is ready to explore these options or needs guidance on finding a suitable detox program, please don’t hesitate. Call our 24/7 helpline at 844-561-0606 for confidential and free assistance.
Promising Therapeutic Targets and Future Directions
The field of addiction medicine is constantly evolving, with researchers diligently working to uncover new and more effective ways to manage opioid withdrawal and prevent relapse. Our understanding of the complex neurobiological mechanisms involved in signs, symptoms, and withdrawal (consolidated) is paving the way for innovative treatments.
Promising areas of research and potential therapeutic targets include:
- Targeting Stress Systems (CRF Antagonists): Given the significant role of the brain’s stress systems, particularly Corticotropin-Releasing Factor (CRF), in mediating the negative affective states of withdrawal, medications that block CRF receptors (CRF antagonists) are being investigated. These could potentially alleviate anxiety and dysphoria during withdrawal.
- Dopamine Stabilizers: Since dopamine system dysregulation contributes to anhedonia and reduced motivation, drugs that help stabilize dopamine levels or function are being explored.
- Non-invasive Brain Stimulation (rTMS): Techniques like repetitive transcranial magnetic stimulation (rTMS) are being studied for their potential to modulate brain activity in circuits involved in craving and withdrawal, offering a non-pharmacological approach.
- Neuro-immune Targets: There’s growing interest in the interplay between the brain and the immune system in addiction. Targeting neuro-inflammatory pathways could offer novel avenues for treatment.
- Novel Neurotransmitter Systems: Future research is also delving into other neurotransmitter systems beyond the classical ones, including the kappa opioid receptor, cannabinoid type 1 receptor, adenosine, and orexin systems, all of which have been implicated in various aspects of withdrawal and addiction.
The goal of these advancements is not just to manage acute withdrawal but to normalize the long-term neural circuit alterations that contribute to relapse vulnerability. This scientific pursuit offers immense hope for the future of addiction medicine, aiming to create more comprehensive and personalized treatments that address the root causes of the disorder.
Conclusion: Taking the First Step Towards Healing
We’ve explored the intricate world of signs, symptoms, and withdrawal (consolidated) from opioids, delving into both the distressing physical sensations and the profound emotional turmoil that characterize this challenging experience. We’ve seen how withdrawal is a complex medical condition, deeply rooted in neurobiological adaptations within the brain’s reward, stress, and memory systems. It’s a testament to the brain’s incredible capacity to adapt, but also to its vulnerability when confronted with powerful substances like opioids.
Understanding this process is crucial not only for those struggling but also for their loved ones and healthcare providers. It helps us recognize that addiction is a disease, not a choice, and that the pain of withdrawal is a very real, scientifically-backed phenomenon. The good news is that recovery is not just a possibility; it’s an achievable reality for anyone willing to take the first step.
At Addiction Helpline America, we are dedicated to being your steadfast partner on this journey. We understand the nuances of withdrawal and the overwhelming feeling of not knowing where to turn. That’s why we offer free, confidential, and personalized guidance to help you find the right recovery program custom to your unique needs. Whether you’re in Birmingham, Alabama, or Portland, Oregon, or anywhere in between, our vast network of treatment centers is ready to support you.
Don’t let the fear of withdrawal or the complexity of finding help deter you. You deserve a life free from the grip of addiction, and we are here to help you achieve it. Call us today at 844-561-0606 to start your journey towards healing and lasting recovery.
Our helpline is 100%
free & confidential
If you or someone you care about is struggling with drug or alcohol addiction, we can help you explore your recovery options. Don’t face this challenge alone—seek support from us.
Programs
Resources
Will my insurance
cover addiction
treatment?
We're ready to help
Find the best
drug or alcohol treatment
center
Are you or a loved one struggling with addiction? Call today to speak to a treatment expert.











