Understanding Relapse as Part of the Recovery Journey
Is relapse common in addiction recovery? Yes, relapse is very common and affects a significant portion of individuals in recovery. Here are the key facts:
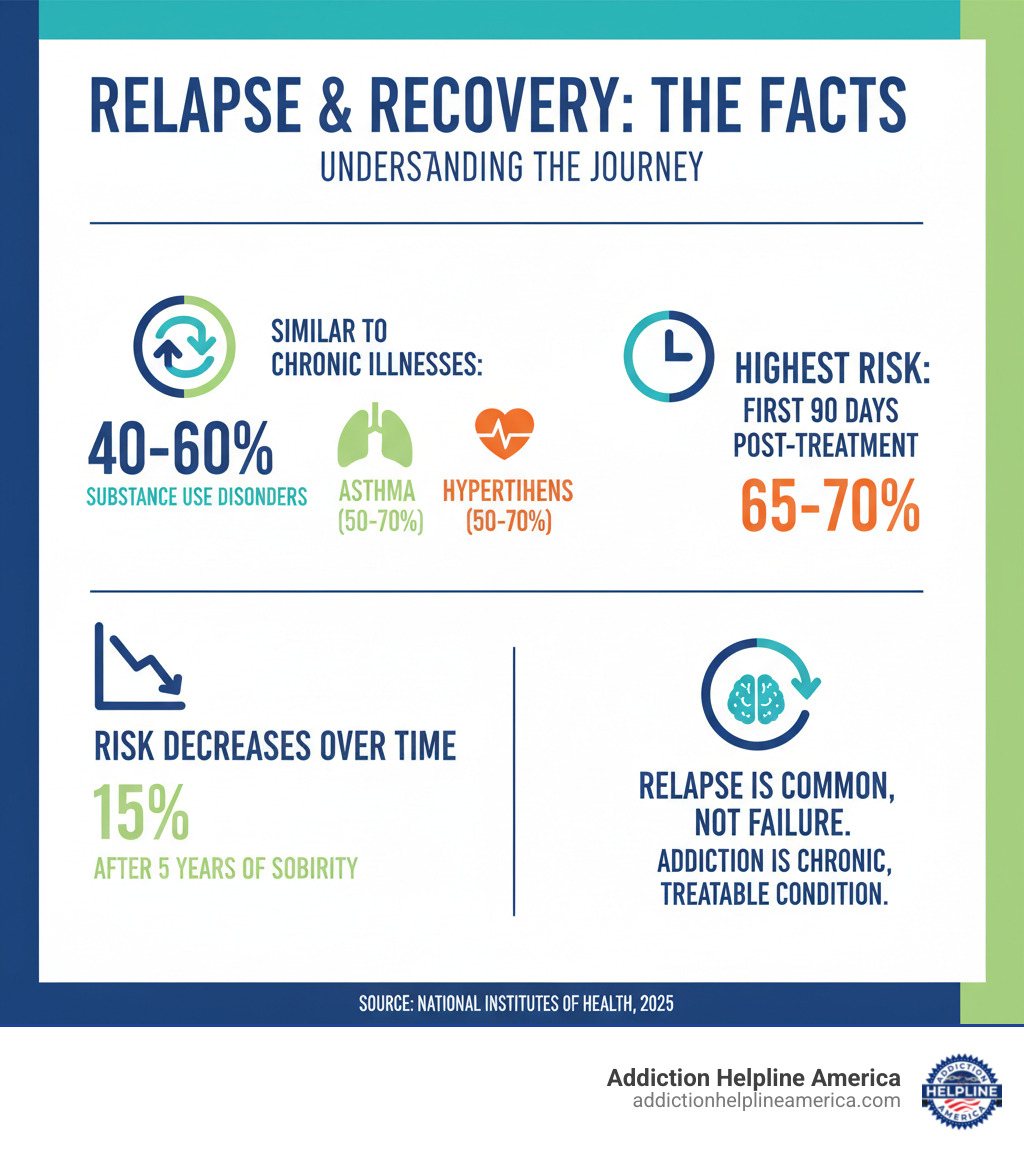
- 40-60% of people treated for substance use disorders will experience relapse at some point
- Relapse rates are similar to other chronic diseases like asthma (50-70%) and hypertension (50-70%)
- More than 85% of individuals may return to substance use within the first year after treatment
- The first 90 days after treatment carry the highest risk, with relapse rates as high as 65-70%
- Risk of relapse decreases significantly over time—dropping to about 15% after five years of continuous sobriety
When you go through the difficult recovery journey and come out on the other side clean and sober, you have a lot to feel good about. Yet you may also feel something many others who have walked in your shoes feel: fear of relapsing.
This fear is understandable. The statistics show that relapse is not just possible—it’s a common part of the recovery process for many people. But here’s what’s important to understand: relapse does not mean failure. It’s not a sign that you’re weak or that treatment didn’t work. Instead, it signals that your recovery plan may need adjustment or reinforcement.
Addiction is a chronic disease, much like diabetes or heart disease. Just as someone with diabetes might have periods where their blood sugar spikes despite following their treatment plan, someone in recovery from addiction may experience a return to substance use. The brain changes that occur with chronic substance use create persistent challenges that require ongoing management.
The good news? Understanding relapse—its causes, warning signs, and prevention strategies—can dramatically improve your chances of long-term recovery. Research shows that the longer you stay in recovery, the lower your risk becomes. Most importantly, each attempt at sobriety builds skills and resilience that strengthen your foundation for lasting change.
At Addiction Helpline America, we’ve supported countless individuals and families navigating the complex journey of addiction recovery, including helping them understand that is relapse common in addiction recovery and developing effective strategies to prevent and manage it. We’re here to provide the compassionate, evidence-based guidance you need at every stage of your recovery journey.
What Is Relapse and Why Isn’t It a Failure?
Let’s start with the basics. Relapse in addiction recovery happens when someone returns to using substances after a period of abstinence. It’s that moment when the disease of addiction resurfaces, pulling a person back into old patterns of use.
But here’s something important to understand: not every slip is the same. There’s a real difference between what we call a “lapse” and a full “relapse.”
Call Now – Your Journey to Recovery Begins Today!

Take the first step towards a healthier life! Call now to connect with our compassionate team and start your recovery journey today. Your path to healing awaits!
Our recovery specialists are available 24/7 to provide support, and all calls are confidential and free. Reach out anytime – we’re here to help!
Think of a lapse as stumbling on your path—a brief, temporary slip. Maybe you have one drink at a wedding or use once in a moment of weakness, but then immediately recognize what happened and get right back on track with your recovery goals. It’s a single instance, not a pattern.
A relapse, on the other hand, is more significant. It’s when that stumble turns into falling back into problematic use. Instead of catching yourself after one slip, you continue using, often escalating back to previous levels or beyond.
| Feature | Lapse | Relapse |
|---|---|---|
| Definition | A single, brief, or minimal use of a substance after abstinence. | A full return to problematic substance use after a period of recovery. |
| Duration | Short-lived; often immediately followed by a return to abstinence. | Prolonged; marks a significant departure from recovery goals. |
| Consequences | Typically less severe; can serve as a warning sign. | More severe; often leads to a full return to addiction. |
| Mindset | Recognizes the slip and recommits to sobriety. | May involve a sense of defeat, leading to further use. |
| Opportunity | An immediate chance to learn and reinforce coping strategies. | An opportunity to reassess and adjust the entire treatment plan. |
Now here’s the crucial part: Is relapse common in addiction recovery? Yes—and understanding why helps remove the shame around it.
Addiction isn’t a character flaw or a lack of willpower. It’s a chronic disease that fundamentally changes how your brain works. The science of addiction as a chronic illness shows us that long-term substance use alters brain chemistry in areas that control pleasure, motivation, stress response, cravings, and impulse control. These changes don’t just disappear when someone stops using—they create lasting challenges that require ongoing management.
Think about other chronic diseases for a moment. If someone with asthma has an attack despite following their treatment plan, we don’t call them a failure. If someone with diabetes experiences a blood sugar spike, we don’t shame them. Instead, we look at what triggered the episode and adjust their treatment approach.
Recovery from addiction works the same way. When relapse happens, it’s not proof that you’re weak or that treatment didn’t work. It’s a signal that something in your recovery plan needs adjustment—maybe additional support, different coping strategies, or a new approach altogether.
This perspective shift is powerful. As explained in Why relapse isn’t a sign of failure, viewing relapse as a learning opportunity rather than a shameful failure is essential for continued progress and long-term sobriety. It’s your chance to understand what went wrong, identify triggers you didn’t know you had, and strengthen the coping mechanisms that will carry you forward.
At Addiction Helpline America, we’ve walked alongside countless individuals through every stage of recovery, including the difficult moments when relapse occurs. We understand that setbacks don’t erase progress—they’re often the stepping stones to stronger, more sustainable sobriety.
So, Is Relapse Common in Addiction Recovery? The Statistics
If you’re wondering “is relapse common in addiction recovery?”—the honest answer is yes. The data tells us clearly that relapse is not only common, it’s actually part of the typical recovery journey for many people. Understanding these statistics can help remove the shame and surprise if it happens to you or someone you love.
The National Institute on Drug Abuse (NIDA) reports that between 40% and 60% of people treated for substance use disorders will experience relapse at some point. That’s nearly half of everyone who goes through treatment. Before you let that number discourage you, consider this: those rates are actually similar to other chronic diseases. People with asthma see symptom recurrence 50% to 70% of the time. The same goes for high blood pressure. This isn’t about willpower—it’s about managing a chronic condition that affects your brain.
The numbers become even more sobering when we look at the first year after treatment. Research shows that more than 85% of individuals may return to substance use within the first year across various types of addiction. Some studies indicate that more than two-thirds of people relapse within just weeks to months after finishing their initial treatment program.
The first 90 days are absolutely critical. This three-month window carries the highest risk, with relapse rates reaching 65% to 70% during this vulnerable period. If you’ve just completed treatment, or you’re supporting someone who has, this is the time when extra vigilance and support matter most.
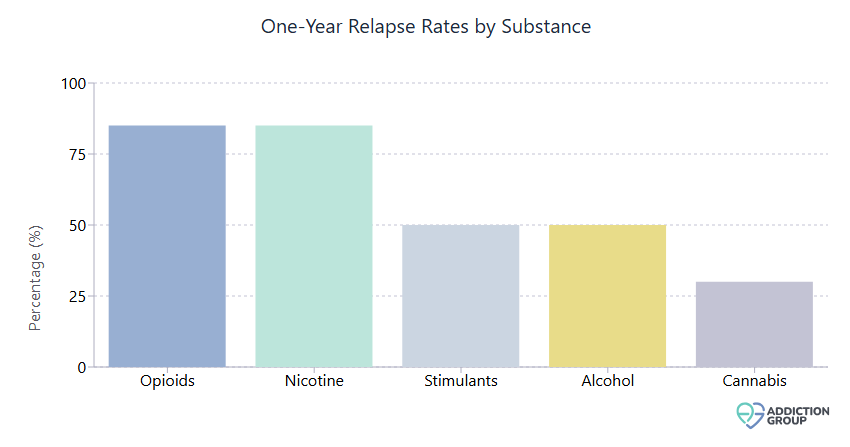
Different substances come with different challenges. Alcohol relapse rates are particularly high—roughly two-thirds of people treated for alcohol use disorder will relapse within the first six months. Over a lifetime, about 90% of individuals with a history of alcohol addiction will experience at least one relapse. But here’s an encouraging fact: for those who make it to five years of sobriety, the annual relapse risk drops dramatically to just 3%.
Opioids present some of the toughest challenges, with relapse rates estimated at 65% to 70% after rehab, and some studies showing rates as high as 91%. Without medication-assisted treatment, a staggering 80% to 90% of people with opioid use disorders may relapse. This is why comprehensive treatment that includes medication options can be so crucial.
For cocaine, approximately 24% of individuals return to weekly use within one year after treatment. Marijuana has its own pattern—about 49% of people seeking help experience a relapse within the first 24 hours if marijuana becomes accessible after treatment. Stimulants like methamphetamine show about a 50% relapse rate within one year, climbing to 75% over five years without ongoing support.
Now for the genuinely good news: relapse rates decrease significantly the longer you stay in recovery. After 12 months of continuous sobriety, your risk begins to drop. By the time you reach five years of continuous sobriety, your odds of long-term success climb to about 85%, with relapse rates generally falling below 15%. Think about that—if you can make it five years, you have an 85% chance of staying sober long-term.
This is why we say recovery is a marathon, not a sprint. Each day, week, and month you stay committed to your sobriety, you’re building momentum and reducing your risk. The statistics aren’t meant to scare you—they’re meant to prepare you, validate your experience, and remind you that if relapse happens, you’re not alone and you’re not a failure. You’re simply facing a challenge that millions of others have faced and overcome.
At Addiction Helpline America, we understand these statistics intimately because we’ve walked alongside countless individuals through every stage of this journey. Whether you’re in your first 90 days or working to strengthen years of sobriety, we’re here to connect you with the support and resources you need.
Call Now – Your Journey to Recovery Begins Today!

Take the first step towards a healthier life! Call now to connect with our compassionate team and start your recovery journey today. Your path to healing awaits!
Our recovery specialists are available 24/7 to provide support, and all calls are confidential and free. Reach out anytime – we’re here to help!
The Relapse Cycle: Triggers, Stages, and Warning Signs
Understanding the journey of recovery means knowing that sometimes, bumps in the road happen. Relapse isn’t usually a sudden event; it’s often a process that unfolds over time, shaped by things both inside and outside of us. These influences are often called “triggers,” and they can start a cycle that, if not addressed, might lead back to substance use.
Think of triggers as little signals or situations that make you more vulnerable. High levels of stress from work, family, or daily life are a big one, as they can make cravings stronger and anxiety higher. Environmental cues are also powerful; these are places, people, objects, or even smells that remind you of past substance use. Going back to old hangouts or seeing old friends who used to use with you can be particularly challenging. Then there are negative emotions like sadness, anger, fear, loneliness, boredom, or feeling resentful. These feelings can overwhelm your ability to cope, making you want to self-medicate. It might surprise you, but even positive emotions or celebrations can be triggers for some. They might think using will make a good mood even better, or that they can “handle” just one drink or drug during a happy occasion.
A simple but powerful reminder is the acronym H.A.L.T. – standing for Hungry, Angry, Lonely, Tired. These physical and emotional states lower your defenses and make you more susceptible to cravings. Recognizing when you’re H.A.L.T. and addressing those needs proactively is a key strategy to stay strong. Other common triggers include interpersonal problems or conflicts with loved ones, which are involved in more than half of all relapses. Physical pain, especially for those who previously used opioids, can also spark a desire for relief. And sometimes, it’s an internal feeling of low self-efficacy – a lack of belief in your own ability to stay sober – that can be a powerful trigger.
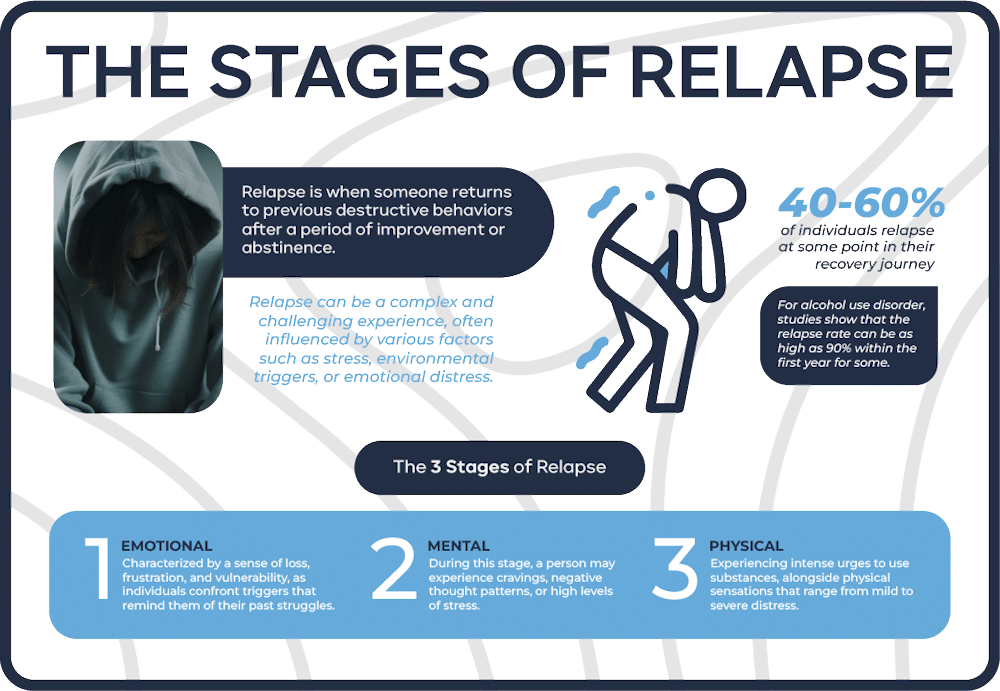
The Three Stages of Relapse
It’s helpful to know that relapse isn’t usually an “on-off” switch. It’s more like a journey that typically moves through three distinct stages: emotional, mental, and physical. Spotting these stages early gives you a chance to step in and prevent a full return to substance use.
The first stage is emotional relapse. Here, you’re not even thinking about using, but your emotions and behaviors are setting the stage for it. You might start bottling up your feelings, pulling away from others, or neglecting self-care like eating well or getting enough sleep. Skipping recovery meetings or therapy sessions, becoming easily angered, or not asking for help are all signs that you might be in emotional relapse.
Next comes mental relapse. This is where the internal battle begins. You start to struggle with the idea of using, caught between wanting to stay sober and battling intense cravings. You might find yourself thinking about the substance, even romanticizing past use and forgetting all the bad things that happened because of it. Thoughts about people, places, and things connected to your past use become more frequent. You might even start bargaining with yourself, thinking, “Maybe just one won’t hurt.” Lying or being dishonest about your thoughts or where you’re going can also be warning signs that you’re planning to relapse or looking for chances to use.
Finally, there’s physical relapse. This is the point where the internal struggle has been lost, and you actually start using the substance again.

Warning Signs: How to Know if a Relapse is Coming
Learning to recognize the subtle hints that come before a relapse can truly be a lifesaver. These warning signs often show up as changes in your attitude, how you act, and what you think:
You might notice behavioral changes, such as becoming secretive, restless, or defensive without clear reason. Isolation is another big red flag, where you start pulling away from friends, family, and your support network. You might begin romanticizing past use, talking or thinking fondly of the “good times” with substances, completely forgetting the negative consequences. Poor self-care is common too, meaning you might neglect personal hygiene, healthy eating, exercise, or sleep. Dishonesty can creep in, as you might lie about where you’ve been or how you’re feeling. Skipping support meetings or therapy sessions shows a reduced engagement in your recovery plan. Sometimes, there’s a loss of desire to recover, where you express doubts about staying sober or feel hopeless about the whole process. You might also experience significant mood swings, feeling more depressed or anxious than usual, and you might start neglecting coping tools you’ve learned for stress or cravings.
The Dangers of Relapsing: Is relapse common in addiction recovery?
While is relapse common in addiction recovery is a question often answered with a resounding “yes,” it’s equally important to understand that common doesn’t mean safe. Relapse comes with very serious dangers that everyone in recovery, and their loved ones, should be aware of.
One of the most critical risks is the potential for overdose due to decreased tolerance. After a period of not using, your body’s ability to handle the substance goes down a lot. If you relapse and use the same amount or strength of the substance you used before, your body might not be able to cope, which can lead to a fatal overdose. This is especially true for opioids, where even a small amount can be deadly after a break. It’s why understanding the risk of overdose after relapse is so important, and why having naloxone available for opioid overdoses can save a life.
Beyond the immediate danger of overdose, relapse brings many other risks. Your physical health can suffer greatly; a return to substance use can make existing health problems worse or cause new ones, impacting your organs, immune system, and overall well-being. There are also significant psychological setbacks. Relapse can trigger intense feelings of shame, guilt, and hopelessness, which can deepen depression and anxiety, making it even harder to get back into recovery. Damaged relationships are another painful consequence. The trust built with loved ones during sobriety can be shattered by a relapse, leading to strained family dynamics, lost friendships, and problems at work. And sadly, a return to substance use often brings back the legal and financial problems that were present during active addiction.
How to Get Back on Track and Prevent Future Relapse
If you’ve experienced a relapse, take a deep breath. This moment, as difficult as it feels, doesn’t erase the progress you’ve made or define your future. The question is relapse common in addiction recovery? has already been answered—yes, it happens to many people walking this same path. What matters now is how you respond.
Call Now – Your Journey to Recovery Begins Today!

Take the first step towards a healthier life! Call now to connect with our compassionate team and start your recovery journey today. Your path to healing awaits!
Our recovery specialists are available 24/7 to provide support, and all calls are confidential and free. Reach out anytime – we’re here to help!
Immediate Steps to Take After a Relapse
The hours and days immediately following a relapse are critical. Your actions right now can mean the difference between a brief slip and a prolonged return to active addiction.
First, be honest—with yourself and with at least one person you trust. This might be your sponsor, your therapist, a family member, or a close friend in recovery. Addiction thrives in secrecy and shadows. The moment you shine light on what happened by speaking it out loud, you begin to take back your power.
Next, reach out for help immediately. Don’t wait until tomorrow or until you “feel ready.” Call your sponsor, text your therapist, show up at a meeting, or contact your treatment provider. If you’re still using, make the decision to stop now. Not later today, not tomorrow—now.
Once you’re safe and clear-headed, take time to assess what happened. What were you feeling before you used? Where were you? Who were you with? What thoughts were running through your mind? This isn’t about beating yourself up—it’s about gathering information. Think of yourself as a detective trying to understand the sequence of events that led to this moment.
Here’s something crucial: avoid drowning in shame and guilt. Yes, those feelings will show up—they’re natural. But excessive shame is actually dangerous because it can trigger more use. Instead of thinking “I’m a failure,” try reframing it as “I’m human, and I need to adjust my approach.” Relapse is a common part of the recovery process for many people, and it doesn’t mean your previous sobriety didn’t count or that you’re back at square one.
Finally, re-engage with treatment. Contact your treatment provider or therapist to discuss what happened and work together to revise your recovery plan. This might mean attending more frequent sessions, trying a different therapy approach, joining an intensive outpatient program, or even returning to residential treatment if needed. There’s no shame in needing more support—in fact, recognizing that need shows strength and self-awareness.
Long-Term Relapse Prevention Strategies
Getting back on track after a relapse is one thing; building a sustainable recovery that lasts is another. Long-term prevention requires ongoing commitment and a toolkit of strategies you can draw on when challenges arise.
A relapse prevention plan is your personalized roadmap for navigating high-risk situations. This isn’t just a mental checklist—it should be written down and shared with your support team. Your plan identifies your specific triggers, outlines concrete coping strategies for each one, and lists emergency contacts you can reach out to when cravings hit or life gets overwhelming.
Developing coping skills is essential because stress, negative emotions, and cravings will inevitably arise. The question isn’t whether you’ll face these challenges, but how you’ll respond to them. Healthy coping mechanisms might include exercise (even a 10-minute walk can shift your mood), journaling to process difficult emotions, calling a friend, engaging in a hobby that absorbs your attention, or using breathing exercises when anxiety spikes. The key is having multiple tools in your toolkit because what works on one day might not work on another.
Identifying your triggers is an ongoing process, not a one-time task. As you progress in recovery, new triggers may emerge, or old ones may lose their power. Continuously reflect on what situations, people, places, emotions, and thoughts make you vulnerable to using. Once you’ve identified a trigger, you have two options: avoid it entirely if possible, or develop specific strategies to steer it safely.
Cognitive therapy, particularly Cognitive Behavioral Therapy (CBT), has proven highly effective in relapse prevention. CBT helps you recognize the thought patterns that lead to substance use—thoughts like “I’ve already messed up, so I might as well keep going” or “Just one won’t hurt.” By identifying these thoughts, you can challenge them and replace them with more accurate, helpful thinking. Many treatment programs incorporate CBT, and it’s worth asking your therapist to focus on these skills.
Mindfulness and relaxation techniques offer powerful tools for managing the moment-to-moment experience of cravings and stress. Meditation teaches you to observe your thoughts and cravings without immediately acting on them. Deep breathing exercises can calm your nervous system when you’re triggered. Yoga combines physical movement with mindfulness, helping you reconnect with your body in healthy ways. These practices aren’t about making cravings disappear—they’re about changing your relationship with them so you’re not controlled by them.
Building a Strong Foundation for Sobriety: Is relapse common in addiction recovery?
While is relapse common in addiction recovery, building a strong foundation dramatically reduces your risk over time. Recovery isn’t just about not using substances—it’s about creating an entirely new life that you don’t want to escape from.
Support systems are non-negotiable. Active participation in 12-step programs like Alcoholics Anonymous or Narcotics Anonymous provides structure, accountability, and connection with others who understand exactly what you’re going through. Research consistently shows a strong correlation between regular meeting attendance and long-term sobriety. Even if meetings aren’t your favorite thing, commit to going anyway—especially during the vulnerable first year.
Working with peer support specialists offers unique benefits that professional therapists can’t provide. These individuals have lived experience with addiction and recovery. They’ve walked the path you’re walking, faced the same doubts, and overcome similar obstacles. Their mentorship combines practical advice with genuine empathy because they’ve been exactly where you are.
Family involvement can heal wounds and create a supportive home environment, which is crucial when you’re fighting to stay sober. Family therapy helps your loved ones understand addiction as a disease, teaches them how to support your recovery without enabling, and provides a space to address past hurts and rebuild trust. Recovery affects the whole family system, and healing those relationships strengthens everyone.
Building a new sober life means making intentional changes to your daily routine and social circle. You’ll need to avoid people, places, and activities associated with your past substance use—at least initially. This might feel like loss, and that’s okay to grieve. But you’re not just giving things up; you’re making space for new friendships, healthier activities, and interests you may have abandoned during active addiction. What did you love before substances took over? What have you always wanted to try? Now is the time.
Service work—helping others in recovery—offers profound benefits for your own sobriety. When you sponsor someone, volunteer at a treatment center, or simply show up for a struggling friend in recovery, you’re reminded of why you chose this path. Service work improves mood, decreases anxiety and depression, increases self-esteem, and strengthens your sense of purpose. It’s hard to think about using when you’re focused on being the person someone else needs.
Relapse Prevention for Co-Occurring Disorders
If you’re managing both addiction and mental health challenges—what’s called a dual diagnosis—relapse prevention requires additional attention. Conditions like depression, anxiety, PTSD, or bipolar disorder significantly complicate recovery and increase relapse risk.
The dual diagnosis challenge is that mental health symptoms often trigger substance use. When you’re struggling with overwhelming anxiety, persistent depression, or intrusive traumatic memories, the urge to self-medicate can feel irresistible. This creates a cycle where substance use temporarily relieves mental health symptoms but ultimately makes them worse, leading to more use.
Integrated treatment is the gold standard for co-occurring disorders. This approach treats your substance use disorder and mental health condition simultaneously through a coordinated team of professionals. Rather than seeing a therapist for depression and a separate counselor for addiction—who may not communicate with each other—integrated treatment ensures all your providers are working together toward the same goals. This comprehensive approach addresses the underlying issues driving your substance use, making long-term recovery more achievable.
Medication management often plays a vital role in dual diagnosis treatment. Working with a psychiatrist to find the right medication and dosage can stabilize your mood, reduce anxiety, manage PTSD symptoms, or balance the brain chemistry affected by bipolar disorder. When your mental health symptoms are properly managed, the urge to use substances as a coping mechanism decreases significantly. It’s important to be open with your doctor about your addiction history so they can prescribe medications with lower abuse potential.
Strategies for mental health and substance use include specialized therapies adapted specifically for dual diagnosis. Cognitive Behavioral Therapy (CBT) can be modified to address both addictive thinking and the cognitive distortions that fuel depression or anxiety. Dialectical Behavior Therapy (DBT) teaches emotional regulation skills that help you manage intense feelings without turning to substances. These therapeutic approaches give you practical tools for navigating the unique challenges of co-occurring disorders.
At Addiction Helpline America, we understand that recovery looks different for everyone, especially when mental health challenges are part of the picture. We connect you with treatment programs that specialize in dual diagnosis, ensuring you receive the comprehensive, coordinated care you need to address all aspects of your health. Because when both conditions are treated effectively, your chances of lasting recovery improve dramatically.
Call Now – Your Journey to Recovery Begins Today!

Take the first step towards a healthier life! Call now to connect with our compassionate team and start your recovery journey today. Your path to healing awaits!
Our recovery specialists are available 24/7 to provide support, and all calls are confidential and free. Reach out anytime – we’re here to help!
Conclusion: Relapse is a Part of the Journey, Not the End of the Road
So, is relapse common in addiction recovery? The answer is unequivocally yes. Throughout this article, we’ve explored the evidence showing that relapse affects 40-60% of people in recovery—rates that mirror other chronic diseases like diabetes or asthma. We’ve seen that the first year, particularly those critical first 90 days, carries the highest risk. We’ve learned that different substances present different challenges, and that triggers can come from stress, environmental cues, emotions, and even positive experiences.
But here’s what matters most: relapse is not the end of your story.
Recovery is not a straight path. It’s not a simple journey from point A to point B where you never stumble or look back. It’s more like climbing a mountain—sometimes you take a few steps backward before finding your footing again. Sometimes you need to rest, reassess your route, and try a different approach. And that’s okay. That’s human.
The science tells us that addiction fundamentally changes the brain, creating a chronic condition that requires ongoing management. When we understand this, we can finally let go of the shame and guilt that so often accompany a return to substance use. Just as we wouldn’t judge someone with diabetes for having a blood sugar spike, we shouldn’t judge ourselves or our loved ones for experiencing a relapse. Instead, we can view it as valuable information—a signal that something in the treatment plan needs adjustment, that new coping skills need to be developed, or that additional support is required.
The truly hopeful message in all the statistics is this: recovery becomes stronger over time. While early recovery is vulnerable, those who maintain sobriety for five years see their relapse risk drop to just 15%. Every day you stay committed to your recovery, you’re building resilience, learning new skills, and creating a life that supports your sobriety. Each challenge you overcome—whether it’s resisting a trigger, reaching out for help when you’re struggling, or getting back up after a fall—makes you stronger for the next one.
Recovery is about progress, not perfection. It’s about taking control of your journey, one day at a time, with compassion for yourself and hope for tomorrow.
At Addiction Helpline America, we’ve walked alongside countless individuals and families through every stage of this journey. We’ve seen people rebuild their lives after multiple relapses. We’ve watched them find strength they didn’t know they had. We’ve celebrated with them as they reached milestones they once thought impossible. And we’ve learned that with the right support, personalized guidance, and evidence-based treatment, long-term sobriety isn’t just a dream—it’s an achievable reality.
Whether you’re just starting your recovery journey, you’re supporting someone you love, or you’re working to get back on track after a relapse, you don’t have to steer this path alone. We provide free, confidential, personalized guidance to connect you with addiction and mental health treatment centers that fit your unique needs. We serve individuals across all fifty states and understand that finding the right program can make all the difference in your success.
If you’re ready to take the next step, or if you simply have questions about recovery, relapse prevention, or treatment options, we’re here for you. Find a confidential relapse prevention program today and find that hope, healing, and lasting sobriety are within your reach. Your story isn’t over—in fact, the best chapters may still be ahead.
Our helpline is 100%
free & confidential
If you or someone you care about is struggling with drug or alcohol addiction, we can help you explore your recovery options. Don’t face this challenge alone—seek support from us.
Programs
Resources
Will my insurance
cover addiction
treatment?
We're ready to help
Find the best
drug or alcohol treatment
center
Are you or a loved one struggling with addiction? Call today to speak to a treatment expert.














