Understanding How IOP Programs Support Recovery
An iop program is a structured treatment approach that helps people recover from addiction and mental health challenges while still living at home and maintaining their daily responsibilities. Here’s what you need to know:
Quick Overview of IOP Programs:
- What it is: A Level 2 treatment program requiring 9+ hours of therapy per week, typically 3-5 days per week
- Who it’s for: People with mild to moderate substance use or mental health issues who have completed detox and have a stable home environment
- What you get: Group therapy, individual counseling, family support, medication management, and life skills training
- Duration: Usually 8-12 weeks, though some programs last 90 days or more
- Cost: Generally $3,000-$10,000 without insurance, but most insurance plans cover IOP as an essential health benefit
- Flexibility: Evening and weekend sessions available so you can work or attend school during treatment
If you or someone you love is struggling with addiction, an IOP program might be the bridge between crisis care and full independence. These programs offer intensive support without requiring you to pause your life. You’ll attend structured therapy sessions several times a week, learn proven recovery skills, and build a support network—all while sleeping in your own bed and maintaining your job or education.
The research is clear: IOPs work. Studies show that people in intensive outpatient programs experience significant improvements in anxiety, depression, PTSD, sleep problems, and overall life satisfaction. These gains last long after the program ends. In fact, 98% of IOP participants say they would recommend the program to others facing similar challenges.
At Addiction Helpline America, we’ve helped thousands of individuals and families steer the path to recovery through programs like IOPs. Our free, confidential service connects you with the right level of care for your unique situation, whether you’re just starting to seek help or transitioning from a higher level of treatment.
Basic iop program vocab:
What is an Intensive Outpatient Program (IOP)?
An Intensive Outpatient Program, or iop program, is a dynamic and flexible treatment option designed to provide comprehensive support for individuals struggling with mental health disorders and substance use challenges. Unlike inpatient treatment, which requires living at a facility, an IOP allows you to receive intensive therapy while continuing to live at home, attend work or school, and engage with your family and community.
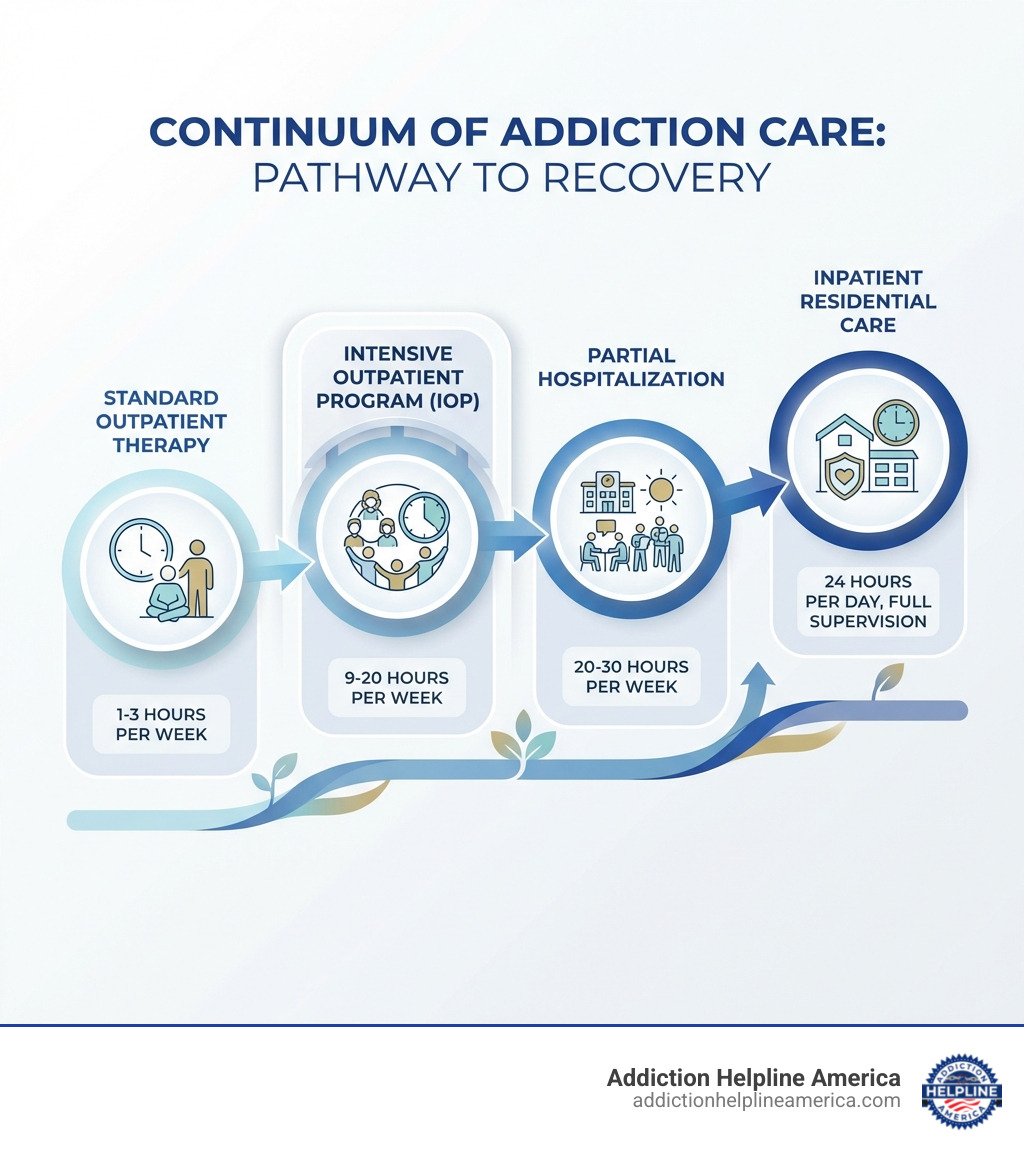
Behavioral health experts rank IOPs as a “Level 2” treatment option within the continuum of care, as defined by the ASAM Criteria for treatment levels. This means an IOP offers a more structured and intensive level of care than standard outpatient therapy, but it’s less restrictive than inpatient or residential treatment. It’s often a crucial stepping stone:
- A step-down from inpatient care: For those transitioning out of a residential program, an IOP provides continued support as they reintegrate into their daily lives.
- A step-up from standard outpatient care: If weekly therapy sessions aren’t providing enough support, an IOP can offer the increased intensity needed to make significant progress.
The core benefit of an IOP is its ability to blend robust clinical care with real-world responsibilities. It’s an ideal solution for individuals who need consistent, structured therapy but have stable housing and a supportive home environment, and do not require 24/7 medical supervision or detoxification.
Key Differences Between an IOP and Other Levels of Care
Understanding where an iop program fits within the spectrum of care is essential:
- Inpatient Treatment / Residential Care: This is the most intensive level, requiring you to live at a facility for the duration of treatment. You receive 24/7 medical monitoring and supervision in a highly structured, substance-free environment. This is typically for individuals with severe addiction, co-occurring mental health disorders requiring constant supervision, or those needing medical detoxification.
- Partial Hospitalization Programs (PHPs): PHPs are often considered a step below inpatient care but more intensive than IOPs. While you return home each day, PHPs typically involve treatment for 6 or more hours per day, most days of the week, offering a highly structured environment without overnight stays.
- Standard Outpatient Therapy: This is the least intensive level of care, usually involving individual or group therapy sessions for a few hours, 1 to 3 times per week. It’s suitable for individuals with mild symptoms or those in the later stages of recovery who need ongoing maintenance and support.
Here’s a quick comparison:
| Feature | Standard Outpatient Program | Intensive Outpatient Program (IOP) | Inpatient/Residential Treatment |
|---|---|---|---|
| Hours/Week | 1-3 hours | 9-20 hours | 24/7 care |
| Living Situation | Lives at home | Lives at home | Lives at facility |
| Intensity | Low | Moderate to High | Very High |
| Cost (without insurance) | Lower | Moderate ($250-$600/week) | Highest |
The Core Benefits of Choosing an IOP
Choosing an iop program offers a unique blend of advantages that can significantly empower your recovery journey:
- Practice Recovery Skills in Real Life: One of the most powerful aspects of an IOP is the opportunity to immediately apply the coping strategies and life skills you learn in therapy to your daily life. This real-world practice helps solidify new behaviors and build confidence in navigating triggers and challenges outside of the treatment setting.
- Build a Strong Support Network: IOPs heavily emphasize group therapy, allowing you to connect with peers who share similar experiences. This shared journey fosters empathy, reduces feelings of isolation, and helps you build a vital support network that can last long after the program ends.
- Cost-Effective Treatment: Compared to inpatient or residential programs, IOPs are generally more affordable, as they don’t include the costs of room and board. This can make high-quality, intensive treatment accessible to more people.
- Flexibility for Work or School: IOPs are specifically designed to accommodate your existing schedule. Many programs offer sessions in the mornings, afternoons, or evenings, allowing you to continue with your job, education, or family responsibilities without interruption. This flexibility removes a significant barrier to seeking help.
- Structured Environment for Healing: While you’re living at home, the program itself provides a consistent, structured routine that can be incredibly beneficial for establishing healthy habits and maintaining accountability during recovery.
- Comprehensive Mental Wellness Support: IOPs don’t just focus on addiction; they often integrate mental health care, providing a holistic approach to your well-being. For more information on comprehensive support, explore our Guide to mental wellness support.
What to Expect from an IOP Program
Engaging in an iop program means committing to a structured yet flexible path toward healing. When you join an IOP, you’re not just attending sessions; you’re becoming part of a supportive community dedicated to growth and recovery.
You can expect to receive an individualized treatment plan custom to your unique needs, challenges, and goals. This plan will guide your daily activities within the program, which typically include a combination of group therapy, individual counseling, family sessions, and educational workshops. The focus is always on developing healthy coping mechanisms, building strong support systems, and equipping you with effective relapse prevention strategies.
What Does a Typical IOP Program Schedule Look Like?
The schedule for an iop program is designed to be intensive enough to be effective, yet flexible enough to allow for your daily life.
- Time Commitment: IOPs generally require participants to attend treatment for at least 9 hours per week. This can be structured in various ways, but a common model involves 3, 3-hour sessions spread across the week. Some programs may offer up to 20 hours of participation per week, depending on individual needs and program design.
- Frequency: You can expect to attend sessions 3 to 5 days a week. Many programs schedule sessions in the mornings or evenings to accommodate work, school, or family obligations.
- Session Length: Individual sessions typically last around an hour, while group therapy sessions can range from 2 to 4 hours.
- Program Duration: The length of an IOP varies based on your progress and needs. While some programs are designed for 4-6 weeks, many last 8-12 weeks, and some individuals may participate for 90 days or more. Your treatment team will regularly assess your progress to determine the most appropriate duration for your recovery journey. For those interested in longer-term structured care, we offer more information in our More info about 90-day rehabs.
Therapies and Interventions Used in IOPs
A key strength of an iop program is its multi-faceted approach to therapy, drawing on evidence-based practices to promote lasting change. You’ll engage in a variety of therapeutic modalities, including:
- Group Therapy: This is often the cornerstone of an IOP. Group sessions provide a safe space to share experiences, receive feedback, and develop social skills in a supportive environment. It fosters a sense of community and reduces feelings of isolation. For a deeper dive into this vital component, read our Complete guide to group therapy.
- Individual Counseling: One-on-one sessions with a licensed therapist allow you to explore personal issues in depth, address underlying trauma, set individual goals, and develop personalized coping strategies.
- Family Therapy: Involving loved ones in the recovery process is crucial. Family counseling sessions help heal relationships, improve communication, and educate family members on how to best support your recovery.
- Cognitive Behavioral Therapy (CBT): This widely used therapy helps you identify and change negative thought patterns and behaviors that contribute to substance use or mental health issues.
- Dialectical Behavior Therapy (DBT): DBT focuses on teaching skills for managing emotions, coping with stress, improving relationships, and living in the present moment. It’s particularly effective for individuals with intense emotional dysregulation.
- Motivational Interviewing (MI): This client-centered approach helps you explore and resolve ambivalence about change, strengthening your motivation for recovery.
- 12-Step Facilitation: Many IOPs integrate principles from 12-Step programs like Alcoholics Anonymous (AA) or Narcotics Anonymous (NA), familiarizing you with these self-help models and encouraging community involvement.
These interventions are designed to equip you with practical tools for navigating life’s challenges sober and with improved mental well-being. For a comprehensive look at clinical issues in intensive outpatient treatment, refer to the SAMHSA guide on clinical issues in IOP.
The Role of Family Involvement
Family involvement plays a critical role in the success of an iop program. Addiction and mental health challenges don’t just affect the individual; they impact entire family systems. Recognizing this, many IOPs integrate family-focused components:
- Family Counseling Sessions: These sessions provide a safe space for family members to communicate openly, address past hurts, and work towards healing relationships.
- Educational Groups for Families: Loved ones often benefit from learning about addiction, mental health disorders, and the recovery process. These groups provide valuable information and strategies for supporting their family member without enabling harmful behaviors.
- Building a Supportive Home Environment: Through family involvement, the goal is to create a home environment that actively supports sobriety and mental wellness, free from triggers and conducive to healthy living.
- Healing Relationships: Recovery is a journey of rebuilding. Family therapy can help mend strained relationships, fostering understanding, empathy, and forgiveness.
- Communication Skills: Participants and their families learn healthier ways to communicate, express needs, and resolve conflicts, which are essential for long-term stability and well-being.
Who Can Benefit from an IOP?
An iop program is not a one-size-fits-all solution, but it is an incredibly effective option for a specific profile of individuals ready to accept change.
The ideal candidate for an IOP is someone who:
- Has a Stable Home Environment: You need a safe, supportive living situation that doesn’t pose an immediate threat to your sobriety or mental well-being.
- Possesses Motivation for Recovery: While motivation can fluctuate, a general willingness to engage in treatment and make changes is crucial.
- Does Not Require Medical Detoxification: IOPs are not equipped for acute withdrawal symptoms. If you need detox, it must be completed before entering an IOP.
- Has Manageable Physical and Mental Health Conditions: While IOPs treat a range of conditions, you should not be at immediate risk of acute intoxication or require 24/7 supervision for severe mental health symptoms. You can manage your symptoms in an outpatient setting but need regular check-ins.
- Needs More Support Than Standard Outpatient: If traditional weekly therapy isn’t enough, but you don’t need the intensity of inpatient care, an IOP is a perfect middle ground.
- Has Reliable Transportation: Consistent attendance is key, so access to reliable transportation to and from the facility is important.
Conditions and Disorders Treated in an IOP
IOP programs are versatile and can effectively treat a wide array of conditions, both independently and as part of a dual diagnosis approach:
- Substance Use Disorders (SUDs): This is a primary focus for many IOPs. Whether it’s alcohol use disorder, opioid use disorder, or other substance dependencies, IOPs provide the structured support needed for lasting sobriety. For example, individuals managing heroin withdrawal symptoms after detox can transition to an IOP for ongoing behavioral therapy.
- Depression: IOPs can offer significant relief for individuals struggling with moderate to severe depression, providing consistent therapy and support to improve mood and functioning.
- Anxiety Disorders: From generalized anxiety to panic disorder, IOPs teach coping mechanisms, stress management techniques, and exposure therapies to reduce anxiety symptoms.
- PTSD (Post-Traumatic Stress Disorder): Specialized IOPs can address trauma through therapies like Prolonged Exposure Therapy, helping individuals process traumatic experiences in a safe environment.
- Eating Disorders: Some IOPs specialize in eating disorders, providing intensive therapy, nutritional guidance, and support for developing healthier relationships with food and body image.
- Borderline Personality Disorder: Dialectical Behavior Therapy (DBT), a common modality in IOPs, is highly effective in treating BPD, focusing on emotional regulation and interpersonal skills.
How IOPs Address Co-Occurring Disorders
It’s common for individuals to experience both a substance use disorder and a mental health disorder simultaneously. This is known as a dual diagnosis or co-occurring disorders. Addressing both conditions concurrently is critical for effective, long-term recovery, and iop programs are expertly designed to do just that.
- Integrated Treatment Approach: Instead of treating addiction and mental health separately, IOPs use an integrated approach. This means your treatment plan will simultaneously address how your mental health impacts your substance use, and vice versa. This holistic view is crucial for breaking cycles of self-medication and improving overall well-being.
- Medication Management: Many individuals with co-occurring disorders benefit from medication to manage mental health symptoms (like depression or anxiety) or to aid in addiction recovery (like Suboxone for opioid use disorder). IOPs often include medication management as part of their comprehensive care, with psychiatrists or medical staff overseeing prescriptions and their effectiveness.
- Team of Specialists: IOPs for dual diagnosis typically employ an interdisciplinary team of professionals, including licensed therapists, addiction counselors, nurses, and psychiatrists. This team collaborates to ensure all aspects of your physical and psychological health are addressed. To learn more about this integrated approach, explore our Guide to dual diagnosis treatment. By treating mental health and addiction together, IOPs offer a more complete path to lasting recovery.
Finding, Choosing, and Paying for an IOP
Starting on an iop program is a significant step toward healing, and finding the right fit is crucial. We understand that navigating treatment options can feel overwhelming, but we’re here to help you make an informed decision.
When considering an IOP, it’s important to look beyond just the location. Key factors like program philosophy, types of therapies offered, staff credentials, and aftercare planning are vital. Look for programs with strong accreditations, which indicate adherence to high standards of care. Our priority is connecting you with programs that are not only effective but also compassionate and custom to your specific needs.
How to Find the Right IOP Program
Finding the right iop program means doing a little research and asking the right questions. We recommend the following steps:
- Asking for Referrals: Start by consulting your primary care physician, a mental health professional, or an addiction specialist. They can often provide referrals to reputable IOPs in your area.
- Online Search and Directories: Use online search engines to look for “IOP program near me” or “intensive outpatient treatment [your city/state]”. The SAMHSA’s national treatment locator is an excellent national resource for finding behavioral health services.
- Questions to Ask Providers: When you contact an IOP, don’t hesitate to ask detailed questions:
- What is your program’s philosophy and approach to treatment?
- What specific therapies and interventions do you use?
- What are the credentials and experience of your staff?
- What is the typical duration of your program?
- Do you offer specialized tracks (e.g., for co-occurring disorders, specific populations)?
- How do you involve family members in the treatment process?
- What kind of aftercare planning and support do you provide upon completion of the IOP?
Understanding the program’s philosophy and how they support you post-treatment is just as important as the treatment itself.
Virtual and Telehealth IOP Options
In today’s connected world, access to an iop program has expanded significantly through virtual and telehealth options. This innovation has broken down geographical barriers and increased flexibility for many individuals.
- Increased Accessibility: Virtual IOPs are particularly beneficial for those in rural areas with limited local treatment options or individuals with mobility challenges.
- Scheduling Flexibility: Attending sessions from the comfort of your home or office can make it easier to fit treatment into a busy schedule, reducing the stress of commuting and allowing you to maintain daily routines.
- Technology Requirements: To participate in a virtual IOP, you’ll need a stable internet connection, a private space for sessions, and a device with a camera and microphone.
- Effectiveness of Virtual Care: Research indicates that virtual IOPs can be as successful as in-person care, provided you have a private and reliable setup. Many care providers understand that virtual attendance might be the only option for some individuals to receive essential treatment.
Understanding the Cost and Insurance Coverage
The cost of an iop program is a common concern, but most insurance plans offer coverage.
- Average Cost: Without insurance, the out-of-pocket cost for an IOP can range from $250 to $600 per week, or $3,000 to $10,000 for a full program. This is significantly less than inpatient treatment, which includes room and board.
- Out-of-Pocket Expenses: Even with insurance, you may have deductibles, copays, or coinsurance to consider. Some insurance plans might also have a cap on the number of visits allowed.
- Verifying Your Benefits: We strongly recommend contacting your insurance provider directly to understand your specific coverage for intensive outpatient programs. Our team at Addiction Helpline America can also assist you in verifying your benefits. For detailed guidance, see our How to find rehabs that accept insurance guide.
- Medicaid Coverage: Many state Medicaid programs, especially those with expansion plans, include IOPs as a covered essential health benefit, often with minimal copay.
- Private Insurance: Major private insurance providers like Cigna often cover IOPs when deemed medically necessary. Learn more about your options with our Guide to Cigna insurance for rehab.
The Affordable Care Act mandates that addiction treatment, including IOPs, be covered as an essential health benefit, making treatment more accessible than ever before.
Frequently Asked Questions about IOPs
We know you might have more questions about iop programs. Here are some common inquiries we receive:
How long does an IOP typically last?
The duration of an iop program varies depending on your individual needs, the specific structure of the program, and your progress. While some programs are shorter, many IOPs typically last between 8 to 12 weeks. However, it’s not uncommon for individuals to participate for 90 days or more, especially if they are making significant progress and benefiting from the structured support. The length of treatment is often progress-based, meaning your treatment team will assess your readiness to transition to a lower level of care or aftercare support.
Can I still work or go to school during an IOP?
Yes, absolutely! One of the primary advantages of an iop program is its flexibility, designed specifically to allow you to maintain your daily responsibilities. Many IOPs offer sessions in the mornings, afternoons, or evenings, as well as on specific days of the week, to accommodate work, school, and family schedules. Federal protections, such as the Family and Medical Leave Act (FMLA), can also support your attendance at work or school during treatment, ensuring job security for eligible individuals.
How effective are IOPs?
IOP programs are highly effective for many individuals, with research indicating impressive success rates. Studies have shown that IOPs can be as effective as inpatient treatment for a significant number of people, with success rates often ranging from 60% to 80% when participants complete the full program and consistently engage in aftercare. A 2021 study, for instance, showed that IOP patients experienced significant and clinically meaningful improvement in multiple areas—including anxiety, sleep disturbances, post-traumatic stress, depression, and life satisfaction. These positive outcomes were sustained for up to six months after leaving the IOP. We encourage you to explore this further with research on IOP effectiveness. The key to success often lies in full engagement with the program and commitment to ongoing support post-treatment.
Your Path to Recovery Starts Here
Choosing an iop program can be a transformative step on your journey to lasting recovery and improved mental wellness. It offers a powerful combination of structured therapy, peer support, and the flexibility to maintain your vital daily life. You gain essential coping skills, build a strong support network, and address underlying issues, all while integrating your healing into the real world.
If you’re wondering if an IOP is the right fit for you, taking the first step is often the hardest, but also the most rewarding. At Addiction Helpline America, we are dedicated to providing free, confidential, and personalized guidance. Our compassionate team can help you understand your options, verify your insurance, and connect you with the right intensive outpatient treatment program custom to your unique needs.
Don’t let uncertainty hold you back from the life you deserve. Reach out today, and let us help you find the support you need to thrive. Your path to recovery starts here.
Find the right intensive outpatient treatment program for you
Our helpline is 100%
free & confidential
If you or someone you care about is struggling with drug or alcohol addiction, we can help you explore your recovery options. Don’t face this challenge alone—seek support from us.
Programs
Resources
Will my insurance
cover addiction
treatment?
We're ready to help
Find the best
drug or alcohol treatment
center
Are you or a loved one struggling with addiction? Call today to speak to a treatment expert.