Understanding the Path from Panic to Peace
Panic disorder treatment offers hope and freedom to those trapped in a cycle of overwhelming fear. If you’re seeking relief from panic attacks, here are the most effective treatment options:
Primary Treatment Approaches:
- Cognitive Behavioral Therapy (CBT) – 70-90% effective, with 73% of patients panic-free within 3-4 months
- Medications – SSRIs and SNRIs as first-line options, with 61% of patients panic-free after 6-12 weeks
- Combination Therapy – Often produces the greatest benefit for symptom relief
- Lifestyle Changes – Exercise, stress management, and avoiding triggers like caffeine and alcohol
Panic disorder is more than just experiencing a single panic attack. It’s characterized by recurrent, unexpected panic attacks followed by at least one month of persistent worry about having more attacks or changing your behavior to avoid them. These attacks can strike without warning, bringing a sudden wave of intense fear, physical symptoms like chest pain and difficulty breathing, and an overwhelming sense of losing control.
The good news? Treatment works. With the right support and evidence-based interventions, most people with panic disorder experience significant improvement and can reclaim their lives.
At Addiction Helpline America, we understand the devastating impact that panic disorder can have on individuals and families, especially when it co-occurs with substance use disorders. Our team has extensive experience connecting people with comprehensive panic disorder treatment programs that address both mental health and addiction recovery needs.
Understanding Panic Disorder: Symptoms, Causes, and Diagnosis
Panic disorder can feel like a relentless storm, but understanding its components is the first step toward navigating it. We often hear about “panic attacks,” but what truly defines the disorder, and what makes it different from simply feeling anxious?
The Anatomy of a Panic Attack
A panic attack is a sudden, intense surge of fear or discomfort that reaches a peak within minutes. It’s a “false alarm” where our body’s natural fight-or-flight response kicks in, even when there’s no real danger. Imagine your body preparing to run from a tiger, but you’re just sitting on your couch. That’s a panic attack.
The symptoms are both physical and psychological, making them incredibly frightening.
Physical Symptoms:
- Racing heart (palpitations): Your heart might pound as if you’ve just run a marathon.
- Shortness of breath or feeling of smothering: You might gasp for air, feeling like you can’t get enough oxygen.
- Chest pain or discomfort: This can be so severe it’s often mistaken for a heart attack, leading many to the emergency room.
- Dizziness, lightheadedness, or faintness: The world might spin, or you might feel like you’re about to pass out.
- Sweating: Your palms might get clammy, or you might break into a cold sweat.
- Trembling or shaking: Your hands or entire body might shake uncontrollably.
- Chills or hot flashes: You might feel sudden temperature changes.
- Numbness or tingling sensations (paresthesias): Often felt in the fingers, toes, or around the mouth.
- Nausea or abdominal distress: A churning stomach or feeling sick.
Psychological Symptoms:
- Fear of dying: A profound sense that something terrible is about to happen, including death.
- Feeling of unreality (derealization) or being detached from oneself (depersonalization): The world might seem strange, or you might feel disconnected from your own body.
- Fear of losing control or “going crazy”: A terrifying sensation that you’re losing your mind or control over your actions.
Most panic attacks typically last between 5 and 20 minutes, though some individuals report them lasting up to an hour. While they are frightening, it’s crucial to remember that panic attacks are not physically dangerous and will not cause you to have a heart attack, suffocate, or lose your mind.
From a Single Attack to a Disorder
Experiencing a single panic attack doesn’t automatically mean you have panic disorder. Many people have one or two isolated attacks in their lifetime. Panic disorder is diagnosed when there’s a pattern of these attacks and a persistent worry about them.
According to the Diagnostic and Statistical Manual of Mental Disorders (DSM-5), a diagnosis of panic disorder requires:
- Recurrent, unexpected panic attacks: These attacks come out of the blue, without an obvious trigger.
- At least one month of persistent worry or concern: After experiencing one or more unexpected attacks, you develop a continuous worry about having more attacks, their potential consequences (e.g., losing control, having a heart attack, “going crazy”), or make significant behavioral changes to avoid situations where attacks might occur.
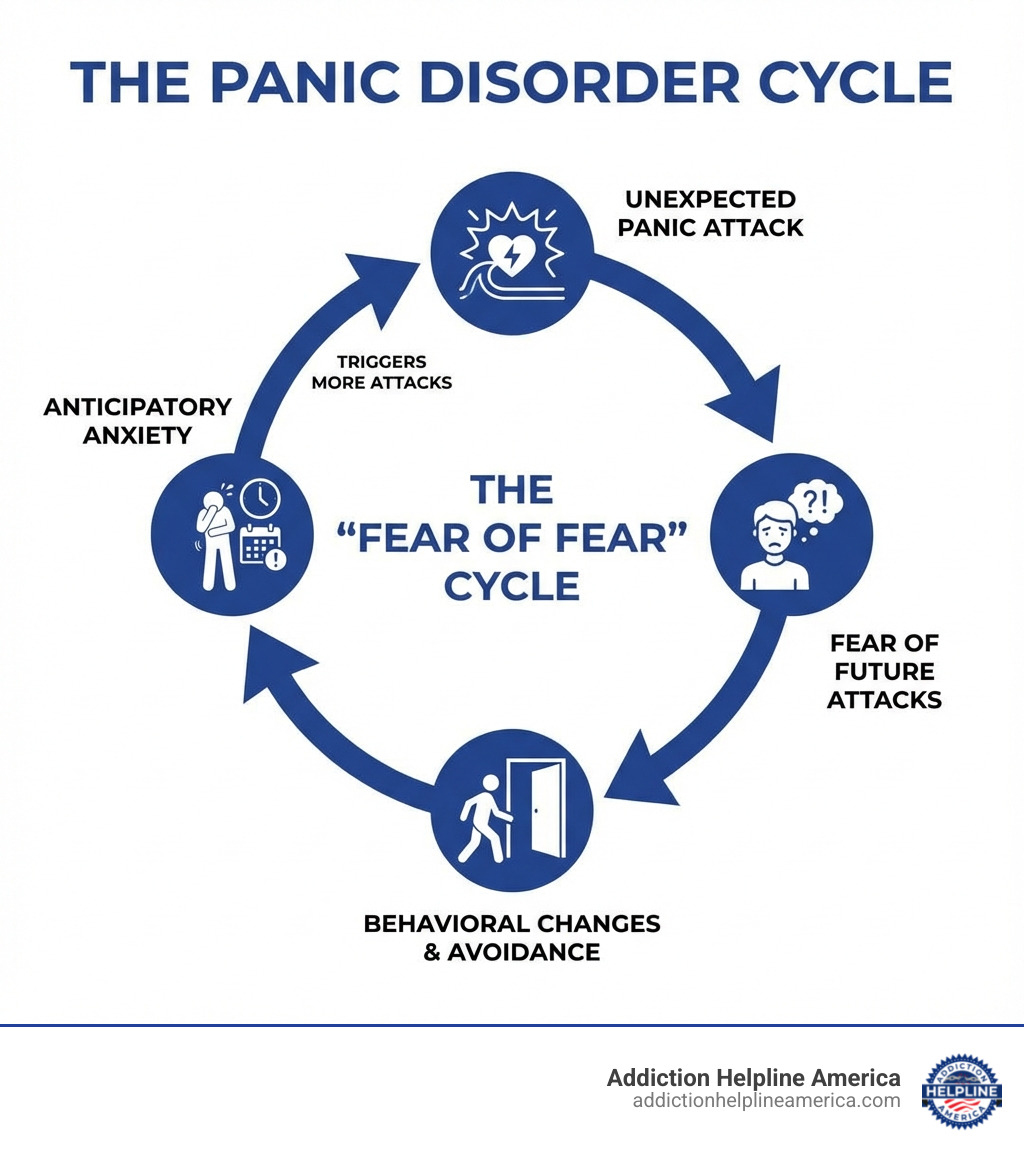
This “fear of fear” cycle is a hallmark of panic disorder. The anticipation of another attack can be as debilitating as the attack itself, leading to avoidance behaviors. For example, if you had a panic attack in a crowded store, you might start avoiding all crowded places. This can escalate into agoraphobia, a type of anxiety disorder where you fear and avoid places or situations that might cause you to panic and feel trapped, helpless, or embarrassed. About one-third of people with panic disorder develop agoraphobia, severely impacting their daily life and independence.
Solving the Causes of Panic Disorder
The exact causes of panic disorder aren’t fully understood, but research suggests a combination of factors contribute to its development. It’s rarely one single cause, but rather a complex interplay.
- Genetic Predisposition: Panic disorder often runs in families, suggesting a genetic link. If a direct family member has panic disorder, you could be up to eight times more likely to develop the condition. If a family member developed it before age 20, the likelihood could increase even further, up to 20 times.
- Brain Chemistry: Researchers believe that imbalances in certain neurotransmitters, such as serotonin, play a role. Dysfunction in brain regions like the amygdala, which processes fear, can also contribute. Panic attacks are sometimes likened to “false alarms” where our survival instincts are overactive.
- Traumatic Life Experiences: Stressful or traumatic events, such as the death of a loved one, a serious accident, or significant life changes, can trigger panic attacks and contribute to the development of panic disorder. Adverse Childhood Experiences (ACEs) can also increase the risk later in life.
- Temperament: Some individuals may have a temperament that makes them more prone to negative emotions or more sensitive to stress.
- Environmental Factors: While not always a direct cause, environmental stressors can certainly exacerbate symptoms.
For more in-depth scientific research on panic disorder, you can visit the National Institute of Mental Health (NIMH) website: Scientific research on panic disorder.
Evidence-Based Panic Disorder Treatment Options
The good news is that panic disorder treatment is highly effective. With the right approach, most individuals can significantly reduce their symptoms and regain control over their lives. Treatment plans are often custom to the individual, considering their unique symptoms, history, and co-occurring conditions.
Therapeutic Approaches for Panic Disorder Treatment
Psychotherapy, often referred to as “talk therapy,” is a cornerstone of effective panic disorder treatment. It helps individuals understand their condition, identify triggers, and develop coping mechanisms.
- Cognitive Behavioral Therapy (CBT): This is the most widely recommended and research-supported psychotherapy for panic disorder. CBT helps us identify and challenge the negative thought patterns and beliefs that fuel panic. It teaches us that while panic symptoms are uncomfortable, they are not dangerous. A key component of CBT for panic disorder is interoceptive exposure, where we deliberately and safely experience the physical sensations associated with panic (e.g., increased heart rate through exercise, dizziness by spinning) to learn that these sensations are not harmful and that we can tolerate them. This process helps to extinguish the “fear of fear.” Through CBT, we learn to:
- Reframe catastrophic thoughts: Instead of thinking “I’m having a heart attack,” we learn to think “This is a panic attack, and it will pass.”
- Develop coping skills: We learn relaxation techniques and strategies to manage physical symptoms.
- Gradually confront feared situations (exposure-based strategies): This helps us reduce avoidance behaviors, like staying home to avoid public places.
CBT is incredibly effective, with studies showing 70 to 90 percent of people who undergo CBT get better. An average of 73 percent of treated patients were panic-free at three to four months in CBT trials. Even self-directed CBT using videotapes and books has shown effectiveness, though less so than standard CBT.
Medications in Panic Disorder Treatment
Medications can be a valuable part of a comprehensive panic disorder treatment plan, especially for managing severe symptoms and allowing individuals to engage more effectively in therapy. They primarily work by affecting brain chemistry to reduce the frequency and intensity of panic attacks and associated anxiety.
- Selective Serotonin Reuptake Inhibitors (SSRIs): These are often the first-line medication choice due to their effectiveness and generally favorable side effect profile. SSRIs, such as fluoxetine (Prozac), paroxetine (Paxil), and sertraline (Zoloft), work by increasing serotonin levels in the brain, which helps regulate mood and anxiety.
- Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs): Medications like venlafaxine (Effexor XR) also increase serotonin, along with norepinephrine, which can further help with anxiety and panic symptoms.
- Tricyclic Antidepressants (TCAs): Older antidepressants like imipramine and clomipramine can also be effective but often have more side effects than SSRIs/SNRIs.
- Benzodiazepines: These anti-anxiety medications, such as alprazolam (Xanax) and clonazepam (Klonopin), provide rapid relief from panic attack symptoms. However, they are typically prescribed for short-term use due to the risk of dependence and withdrawal.
Antidepressant medications take time to work. They can take 2 to 4 weeks to start showing effects, and up to 8 weeks to work fully. With antidepressant treatment, 61 percent of patients were panic-free after six to 12 weeks, compared with 41 percent of control patients. The combination of an antidepressant with some form of CBT often produces the greatest benefit in short-term studies.
Always discuss medication options thoroughly with a healthcare provider. They can help us understand how medications can help manage symptoms and provide professional guidance on the right choice for our specific needs.
Understanding Medication Risks and Side Effects
While medications can be highly beneficial in panic disorder treatment, be aware of their potential risks and side effects. Our healthcare provider will discuss these with us to ensure we make informed decisions.
Short-term and long-term medication considerations:
- SSRIs and SNRIs: Common side effects can include nausea, insomnia, nervousness, headache, and sexual dysfunction. These often subside after the first few weeks. Long-term use is generally considered safe and effective, but discontinuation should always be done under medical supervision to avoid withdrawal symptoms.
- Benzodiazepines: These medications offer quick relief but carry significant risks, including:
- Dependence and tolerance: The body can quickly become accustomed to benzodiazepines, requiring higher doses for the same effect. Dependence can occur in 30% of patients on therapy longer than 8 weeks.
- Withdrawal symptoms: Discontinuing benzodiazepines abruptly can lead to severe withdrawal symptoms, including rebound anxiety, seizures, and increased panic attacks. Tapering off these medications must be done very slowly, often over several months, under medical guidance.
- Sedation and cognitive impairment: They can cause drowsiness, dizziness, and memory problems, impacting daily activities like driving.
- Potential for misuse: Due to their rapid effect, there’s a risk of misuse, especially in individuals with a history of substance abuse.
- TCAs: Side effects can include dry mouth, blurred vision, constipation, urinary retention, and drowsiness. They also have potential cardiac effects, requiring careful monitoring.
It’s crucial to have open communication with our healthcare provider about any side effects we experience. They can adjust dosages, switch medications, or offer strategies to manage side effects. The U.S. Food and Drug Administration (FDA) website is an excellent resource for up-to-date information on medications, side effects, and warnings: Information on medications from the FDA.
Lifestyle Changes and Self-Management Strategies
While professional intervention is key to panic disorder treatment, incorporating lifestyle changes and self-management strategies can significantly improve our progress and empower us to take an active role in our recovery.
In-the-Moment Coping Techniques
When a panic attack strikes, it can feel overwhelming. Having a plan and a few go-to techniques can make a big difference:
- Deep breathing exercises: Focus on slow, deep breaths. Inhale slowly through your nose for a count of four, hold for a count of four, and exhale slowly through your mouth for a count of six. This helps regulate your nervous system.
- Grounding techniques: These help us reconnect with the present moment and distract from the intense internal sensations. The “5-4-3-2-1 method” is popular: identify 5 things you can see, 4 things you can touch, 3 things you can hear, 2 things you can smell, and 1 thing you can taste.
- Acknowledging the attack: Remind yourself, “This is a panic attack, it’s uncomfortable, but it’s not dangerous.” Trying to fight or suppress the attack can sometimes make it worse.
- Self-reassurance: Repeat calming phrases like “This will pass,” “I am safe,” or “I can handle this.” Allow the attack to run its course rather than desperately trying to stop it. Panic attacks usually last less than 10 minutes and are not life-threatening.
Long-Term Lifestyle Adjustments
Beyond immediate coping, consistent healthy habits can reduce the frequency and intensity of panic attacks over time.
- Regular physical exercise: Engaging in physical activity, like walking, jogging, or yoga, can help manage stress, relieve tension, and boost mood. Even a simple 30-minute walk most days of the week can make a difference.
- Stress management: Identify your stressors and find healthy ways to manage them, such as mindfulness, meditation, or spending time in nature. Learning breathing exercises specifically for stress can also be beneficial.
- Healthy diet: A balanced diet supports overall mental and physical health. Avoid sugary foods and drinks that can lead to energy crashes and exacerbate anxiety.
- Sleep hygiene: Prioritize getting enough quality sleep. Establish a regular sleep schedule, create a relaxing bedtime routine, and ensure your sleep environment is conducive to rest.
- Avoiding triggers: Certain substances can worsen panic symptoms. We strongly advise limiting or avoiding:
- Caffeine: Stimulants can mimic panic symptoms like a racing heart.
- Alcohol: While it might seem to provide temporary relief, alcohol can disrupt brain chemistry and lead to worse anxiety and panic attacks, especially as it wears off.
- Smoking: Nicotine is a stimulant and can increase anxiety and the likelihood of panic attacks.
The Power of Connection: Support Systems
We are not alone in this journey. Building and utilizing a strong support system is a powerful element of panic disorder treatment.
- Role of support groups: Connecting with others who understand what we’re going through can be incredibly validating and empowering. Support groups offer a safe space to share experiences, learn coping strategies, and realize that our struggles are not unique. Organizations like the Anxiety and Depression Association of America (ADAA) can help us find local or online support groups.
- How to support a loved one: If someone we care about is experiencing panic disorder, our support is invaluable.
- Educate ourselves: Learn about panic disorder to better understand what they’re going through.
- Communicate openly: Encourage them to share their feelings without judgment.
- Practice patience and compassion: Recovery is a process, not a linear path. Acknowledge their progress and be there for setbacks.
- Offer reassurance: During an attack, remind them they are safe and that the attack will pass.
- Help them seek professional help: Offer to help find a therapist or accompany them to appointments.
For more information on finding support and locating mental health services in your area, the Substance Abuse and Mental Health Services Administration (SAMHSA) website is a valuable resource: Finding support and mental health services.
Frequently Asked Questions about Panic Disorder Treatment
We understand that you likely have many questions about panic disorder treatment. Here, we address some of the most common concerns.
How long does treatment for panic disorder take?
The duration of panic disorder treatment varies significantly from person to person. It’s not a quick fix, but rather a process of healing and learning new coping skills.
- Therapy results: With CBT, some individuals may start to see symptom reduction within several weeks, with significant improvement often occurring within three to four months. However, a full course of therapy might last 12 to 16 sessions or longer, depending on individual needs and the severity of the disorder. The benefits of psychological treatment tend to last the longest.
- Medication timeline: Antidepressants typically take 2 to 4 weeks to start working and up to 8 weeks to reach their full effect. Once symptoms are stable, medication is usually continued for at least six months to a year to prevent relapse.
- Long-term management: For some, treatment may involve long-term maintenance therapy or medication, while others may learn to manage their symptoms effectively and discontinue active treatment. The goal is always to achieve lasting relief and a return to a fulfilling life.
Can panic disorder be cured completely?
While some mental health professionals prefer to speak of “management” rather than a “cure” for panic disorder, the reality is that with effective panic disorder treatment, most people can achieve significant symptom reduction, often to the point of complete remission. The focus is on learning to manage symptoms, understand triggers, and prevent future attacks, allowing individuals to live full, unrestricted lives.
With treatment, the long-term outlook is very positive. The aim is to equip you with the tools and strategies to steer future challenges without the debilitating impact of panic attacks. Relapse prevention is an important part of treatment, helping us identify early warning signs and take action.
Are panic attacks physically dangerous?
This is one of the most common and terrifying fears associated with panic attacks, and we want to be absolutely clear: No, panic attacks are not physically dangerous. They are frightening and uncomfortable, but they will not cause you to have a heart attack, suffocate, or lose consciousness in a way that harms you. Your body’s alarm system is simply overreacting.
However, because the physical symptoms can mimic serious medical conditions (like a heart attack), it’s always wise to consult a healthcare provider if you experience these symptoms for the first time. This ensures that any underlying medical conditions are ruled out. Once medical causes have been excluded, we can be reassured that what we’re experiencing, while terrifying, is not physically harmful.
Take the First Step Towards Freedom
Living with panic disorder can feel like being trapped in a cycle of fear, but we want you to know that freedom is within reach. Panic disorder treatment is highly effective, and with the right support, you can learn to manage your symptoms, regain control, and live the life you deserve. You are not alone in this journey, and countless individuals have successfully steerd their path from fear to peace.
At Addiction Helpline America, we are dedicated to guiding you through this process. We connect individuals nationwide across Alabama, Alaska, Arizona, Arkansas, California, Colorado, Connecticut, Delaware, Florida, Georgia, Hawaii, Idaho, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Montana, Nebraska, Nevada, New Hampshire, New Jersey, New Mexico, New York, North Carolina, North Dakota, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, South Carolina, South Dakota, Tennessee, Texas, Utah, Vermont, Virginia, Washington, West Virginia, Wisconsin, Wyoming, and the District of Columbia, to specialized treatment centers. Our free, confidential, and personalized guidance ensures you find the right recovery program from our vast network, addressing both panic disorder and any co-occurring conditions.
Taking the first step can be the hardest, but it’s the most important. Let us help you take control of your life and start on your journey to lasting well-being.
Our helpline is 100%
free & confidential
If you or someone you care about is struggling with drug or alcohol addiction, we can help you explore your recovery options. Don’t face this challenge alone—seek support from us.
Programs
Resources
Will my insurance
cover addiction
treatment?
We're ready to help
Find the best
drug or alcohol treatment
center
Are you or a loved one struggling with addiction? Call today to speak to a treatment expert.